Glador M, Glimepiride/ Metformin
- Introduction to Glador M
- Composition and Formulation
- Active ingredients: Glimepiride and Metformin Hydrochloride
- Glimepiride Drug Class
- Available Strengths and Dosage Forms
- Excipients and Pharmaceutical Properties
- Glimepiride vs Glipizide
- Glimepiride vs Metformin
- Glyburide vs Glimepiride
- Glimepiride vs Jardiance
- Berberine vs Metformin
- Metformin vs Ozempic
- Jardiance vs Metformin
- Metformin vs Semaglutide
- Farxiga and Metformin
- Mechanism of Action: How Glador M Works
- Approved Medical Uses of Glador M
- Off-Label Uses of Glimepiride/Metformin Combination
- Dosage and Administration Guidelines
- Common and Serious Side Effects of Glador M
- Drug Interactions with Glador M
- Contraindications for Glador M Use
- Warnings and Important Precautions
- Careful Administration and Monitoring Recommendations
- Use in Special Populations
- Overdose and Emergency Management
- Handling and Storage Instructions
- Considerations
Introduction to Glador M
Glador M is an oral medication used to treat Type 2 Diabetes Mellitus (T2DM). It's a combination drug, bringing together two strong medications: Glimepiride and Metformin Hydrochloride. This dual approach tackles the two main problems in T2DM: insulin resistance and issues with the pancreas's beta cells.
Using these two drugs together improves blood sugar control because they work in complementary ways. Glimepiride encourages your body to release more insulin, while Metformin makes your body more sensitive to insulin and reduces the liver's sugar production. This combined effect often means lower doses of each drug are needed, which can reduce side effects.
Glador M is a brand-name drug, but many generic versions are also available. While brand and generic drugs might differ in their inactive ingredients and how well they're absorbed, regulatory bodies ensure they are therapeutically equivalent. Glador M is approved by several national drug agencies, including India's CDSCO, and is made by reputable pharmaceutical companies like Micro Labs and others under license.
Composition and Formulation
Active ingredients: Glimepiride and Metformin Hydrochloride
Glimepiride is a type of third-generation sulfonylurea that helps boost the release of insulin from the beta cells in the pancreas. Metformin Hydrochloride is a medication that helps lower the production of glucose in the liver and boosts the body's ability to absorb glucose peripherally.
Glimepiride Drug Class
Glimepiride is categorized under the sulfonylurea group, which is recognized for its impact on insulin production in the body. It interacts with the SUR1 segment of beta cell membranes, ATP potassium channel leading to membrane depolarization and eventual release of insulin content. Decimal sensitivity compared to sulfonylurea ensures an effect, with a reduced likelihood of hypoglycemia occurring.
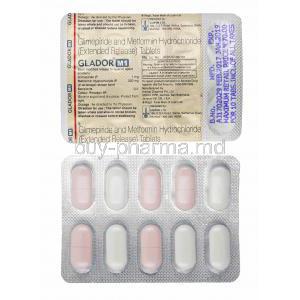
Available Strengths and Dosage Forms
Glador M comes in different strengths to suit individual patient needs:
- Glador M1 contains 1 mg of Glimepiride and 500 mg of Metformin.
- Glador M2 contains 2 mg of Glimepiride and 500 mg of Metformin.
- Depending on local regulations, you might also find both extended-release (ER) and immediate-release (IR) versions.
Excipients and Pharmaceutical Properties
The ingredients in this formulation consist of substances like microcrystalline cellulose and povidone, along with magnesium stearate and hypromellose to improve tablet strength and absorption rates for effectiveness. The tablets are often coated with a film to safeguard against stomach acidity and make swallowing easier.
Glimepiride vs Glipizide
Glimepiride and Glipizide fall under the category of sulfonylureas; however they vary in terms of how they work in the body and their effectiveness. Glimepiride has an affinity to receptors. Stays active for a longer time, making it suitable for once a day usage. In contrast, Glipizide has a shorter impact period. It is typically taken times throughout the day. Doctors might prefer Glimepiride due to its ability to maintain blood sugar levels while causing resistance to insulin.
Glimepiride vs Metformin
This medication combines two approaches to manage blood sugar: it encourages the body to release more insulin and makes the body's cells more responsive to insulin. These two drugs work together to improve blood sugar control effectively, and importantly, they do so without causing significant weight gain, which can be a common side effect when using only sulfonylurea medications.
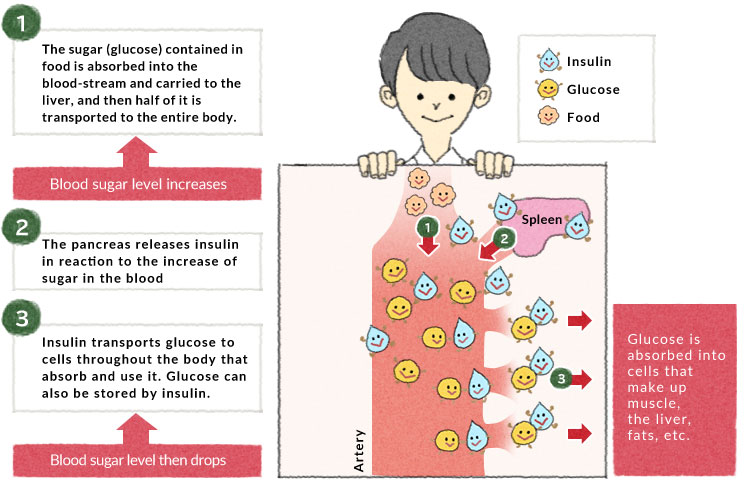
Glyburide vs Glimepiride
The medication Glyburide is also referred to as glibenclamide. Belongs to the generation of sulfonyureas, which pose a higher risk of hypoglycemia and weight gain compared to Glimepiride, offering a safer profile, with less notable fluctuations, in blood sugar levels and a more favorable pharmacodynamic profile.
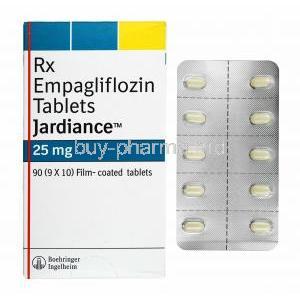
Glimepiride vs Jardiance
Empagliflozin (Jardiance) is an SGLT2 inhibitor that helps lower blood sugar by causing the body to excrete glucose in the urine, and it does so independently of insulin. While Glimepiride is effective for managing blood sugar, especially when cost or immediate glucose control is a priority, Jardiance provides extra benefits for heart and kidney protection.
Berberine vs Metformin
Berberine, a natural compound found in plants, works similarly to Metformin by making the body more sensitive to insulin. Early studies suggest it might be as effective at lowering blood sugar. However, Metformin is still the preferred treatment because it has extensive clinical trial data, a proven safety record, and is more affordable. Berberine's use is currently considered supplementary and is still being researched.
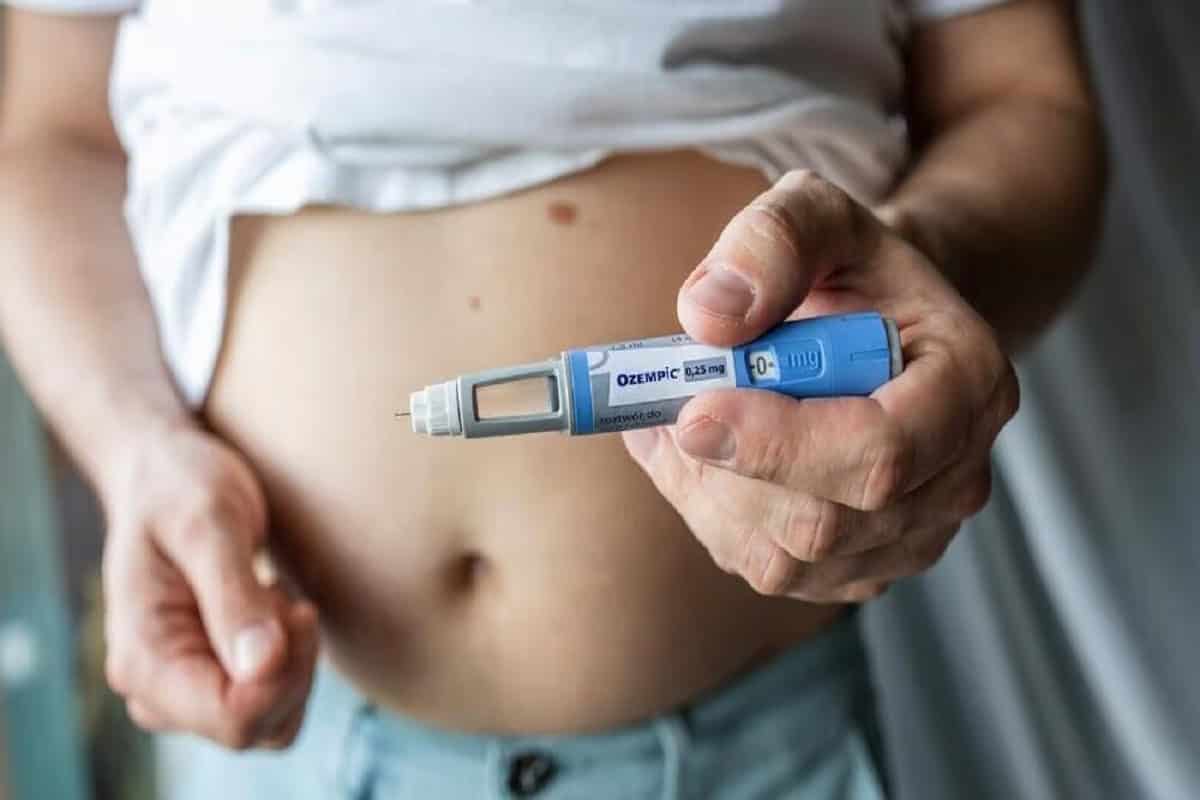
Metformin vs Ozempic
Ozempic (semaglutide), a GLP-1 receptor agonist, has significant effects on weight loss and lowering HbA1c (a measure of average blood sugar). Unlike Metformin, it also slows down digestion and reduces appetite. While Metformin is usually the first choice because it's affordable and has a long history of safe use, Ozempic is becoming a strong second option for patients who need more intensive treatment.
Jardiance vs Metformin
Metformin targets liver insulin resistance while Jardiance works to decrease glucose reabsorption in the kidneys. Jardiance provides advantages like lowering the need for heart failure hospital stays and safeguarding against kidney disease. When used together in combination therapy, these medications create an outcome.
Metformin vs Semaglutide
While Semaglutide, given as a weekly injection, is better than Metformin at lowering blood sugar (HbA1c) and helping with weight loss, it often causes more gastrointestinal side effects and is more expensive. Because of its ease of use and affordability, Metformin remains the go-to choice for initial diabetes treatment.
Farxiga and Metformin
Farxiga (dapagliflozin), when paired with Metformin, focuses on two pathways, for diabetes management. Improving insulin sensitivity. Enhancing glucose excretion. By combining these two medications, it not only effectively lowers HbA1c levels compared to using each drug, but also provides potential benefits for heart and kidney health in individuals dealing with heart failure or chronic kidney disease (CKD).
Mechanism of Action: How Glador M Works
Glimepiride: Sulfonylurea Mechanism and Pancreatic Stimulation
Glimepiride, a type of modern sulfonylurea drug, lowers blood sugar by increasing the amount of insulin released from the pancreas's beta-cells. It does this by strongly attaching to a specific receptor (SUR1) on these cells, which then closes certain potassium channels.
When these channels close, it causes a change in the cell's electrical charge, opening up calcium channels. This rush of calcium into the cell ultimately triggers the release of insulin. The newly released insulin then helps muscles and fat tissues absorb more glucose from the blood.
In summary, Glimepiride primarily:
- Acts on the pancreas to stimulate insulin release.
- Helps with the initial rapid release of insulin.
- Might also have minor effects outside the pancreas that improve insulin sensitivity.
Metformin: Biguanide Action and Hepatic Glucose Production Inhibition
Metformin works differently from other medications. Its main action is on the liver, where it reduces glucose production through a process called gluconeogenesis. It does this by activating an enzyme called AMP-activated protein kinase (AMPk), which then controls the activity of other enzymes involved in glucose production (like PEPCK and glucose-6-phosphatase).
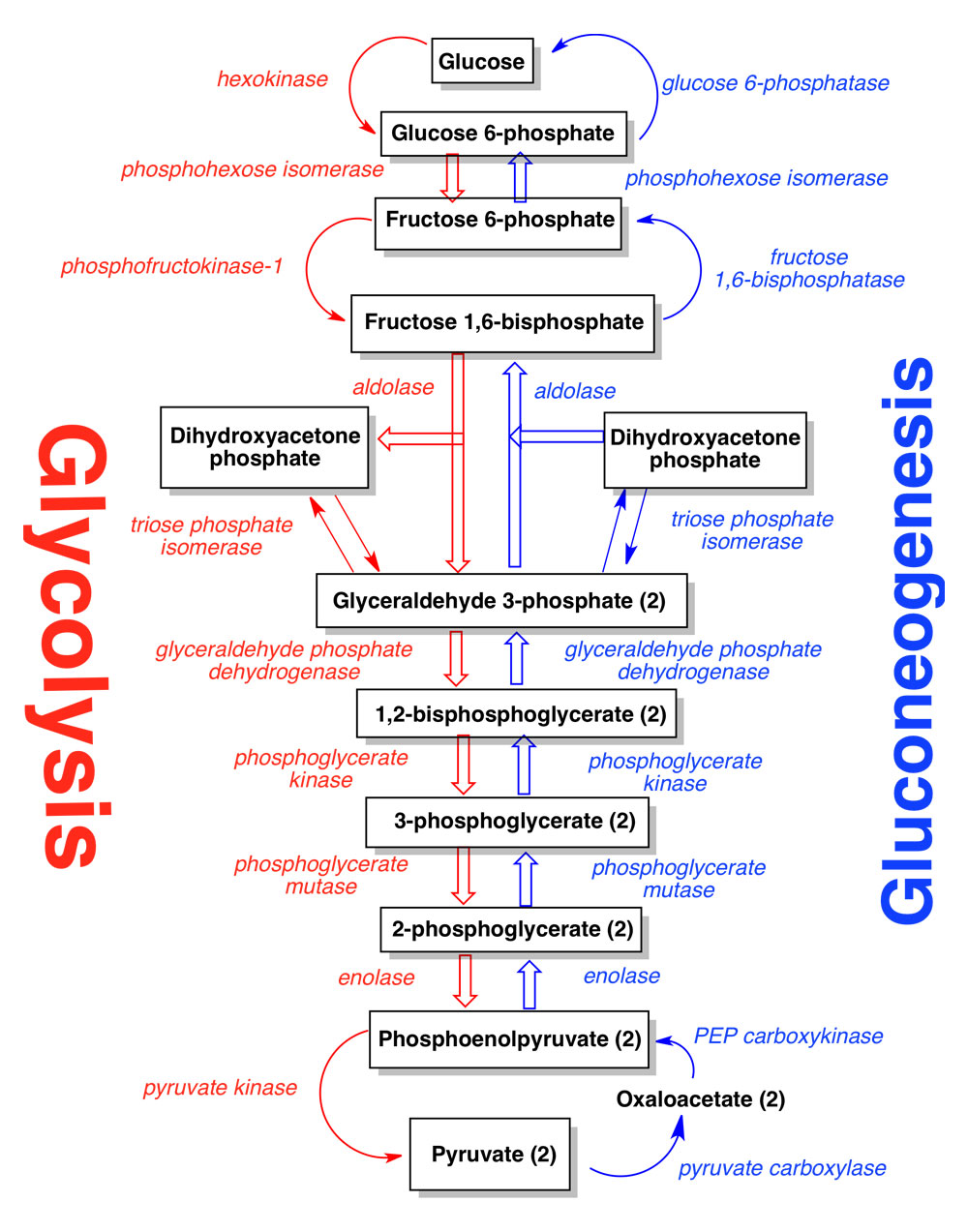
Beyond its liver effects, Metformin also improves how well the body's tissues, especially muscles, respond to insulin. This means your body can better absorb and use glucose. It also positively affects fat metabolism and blood vessel function.
Essentially, Metformin:
- Boosts insulin's ability to help cells take in glucose.
- Doesn't stimulate insulin secretion, which means it rarely causes low blood sugar (hypoglycemia) on its own.
Synergistic Effect in Glycemic Control
The use of Glimepiride and Metformin, in Glador M provides a well-rounded approach to controlling blood sugar levels effectively. Specifically Glimepiride targets the production of insulin while Metformin tackles insulin resistance and excessive glucose production by the liver.
When used simultaneously the combination lowers both fasting and after-meal blood sugar levels efficiently than using each medication.
The diverse ways these medications work allow for doses, per drug reducing the chances of experiencing side effects that are dose dependent. Reduced risk of gaining weight and experiencing blood sugar levels compared to doses of sulfonylureas.
Time to Onset and Duration of Action
Glimepiride starts working within an hour of taking it, reaching its highest levels in the blood in about 2 to 3 hours, and its effects can last for up to 24 hours, making it suitable for once-daily dosing for most patients.
Metformin, on the other hand, takes a bit longer to show its full benefits, usually a few days, with stable blood levels typically achieved within 24 to 48 hours. You'll likely see improvements in blood sugar after about two weeks of use. Although its half-life in the bloodstream is around 4 to 5 hours, its effects last longer because it accumulates in the gut and liver.
In essence:
- Glimepiride generally begins working within an hour and remains effective for 24 hours.
- Metformin usually starts showing effects within 48 hours, with its full benefits typically felt within 7 to 14 days.
- These different action profiles are key to how both medications manage blood sugar, both before and after meals.
Approved Medical Uses of Glador M
First-Line and Second-Line Treatment for Type 2 Diabetes Mellitus
Glador M is recommended for individuals with Type 2 Diabetes Mellitus (T2DM), particularly when lifestyle adjustments alone aren't sufficient. It can serve as an initial treatment for those diagnosed with very high blood sugar (HbA1c of 7.5% or higher) or poorly controlled glucose, especially when immediate action is necessary.
Often, Glador M is prescribed as a subsequent treatment when either Glimepiride or Metformin alone hasn't achieved the desired results. This combination medication effectively targets the core issues of T2DM, leading to improved treatment outcomes and better patient adherence. It's also a valuable option for patients who cannot take other second-line medications like SGLT2 inhibitors
Indications for Dual Therapy in Uncontrolled Diabetes on Monotherapy
Glador M can be a good option for patients who struggle to control their blood sugar with a single medication, or when their condition worsens to the point where they might otherwise need insulin injections. This medication helps manage blood sugar in two ways: by improving the function of beta cells and reducing insulin resistance in the liver. Often, using Glador M can delay the need for insulin therapy and make managing their diabetes feel less overwhelming for patients.
It's particularly useful when:
- HbA1c levels consistently remain above target (e.g., 7.5%) despite lifestyle changes and a single medication.
- There are signs of worsening beta cell function or persistently high fasting blood sugar.
- Patients have restrictions on using other medications like DPP-4 inhibitors or GLP-1 receptor agonists.
Use in Metabolic Syndrome with Insulin Resistance
Beyond treating classic diabetes, Glador M is also useful for patients with metabolic syndrome. This condition involves a cluster of issues like belly fat, unhealthy cholesterol levels, high fasting blood sugar, and high blood pressure. Insulin resistance is the core problem linking these features, often appearing before full-blown diabetes.
In these patients, Metformin works to combat insulin resistance in the liver and other tissues, while Glimepiride boosts the body's own insulin production if the pancreas is still partly functional. This combination acts as a powerful tool to change the course of cardiometabolic disease.
Specifically, Glador M:
- Aids early blood sugar intervention in individuals with high-risk metabolic profiles.
- Enhances insulin sensitivity and improves fat metabolism.
- Decreases inflammatory markers linked to blood vessel problems.
Role in Combination with Lifestyle Modification
For medications to work best, they should always be paired with lifestyle changes, specifically diet adjustments and regular exercise. This combination helps your body's metabolism work more efficiently and keeps blood sugar levels steady, avoiding big ups and downs.
When patients understand and commit to these lifestyle changes, it often means they can take lower doses of medication, which helps minimize potential side effects like episodes of low blood sugar. This combined approach also helps improve cholesterol levels, reduce insulin resistance, and generally boosts overall well-being. Ultimately, it significantly reduces the risk of long-term heart and blood vessel problems.
Off-Label Uses of Glimepiride/Metformin Combination
Use in Polycystic Ovary Syndrome (PCOS)
Although not officially approved for Polycystic Ovary Syndrome (PCOS), the combination of Glimepiride and Metformin has been investigated as an additional treatment for insulin resistance, a key feature of this hormonal disorder. PCOS often involves high insulin levels, irregular ovulation, and excess male hormones, all contributing to fertility issues and metabolic problems.
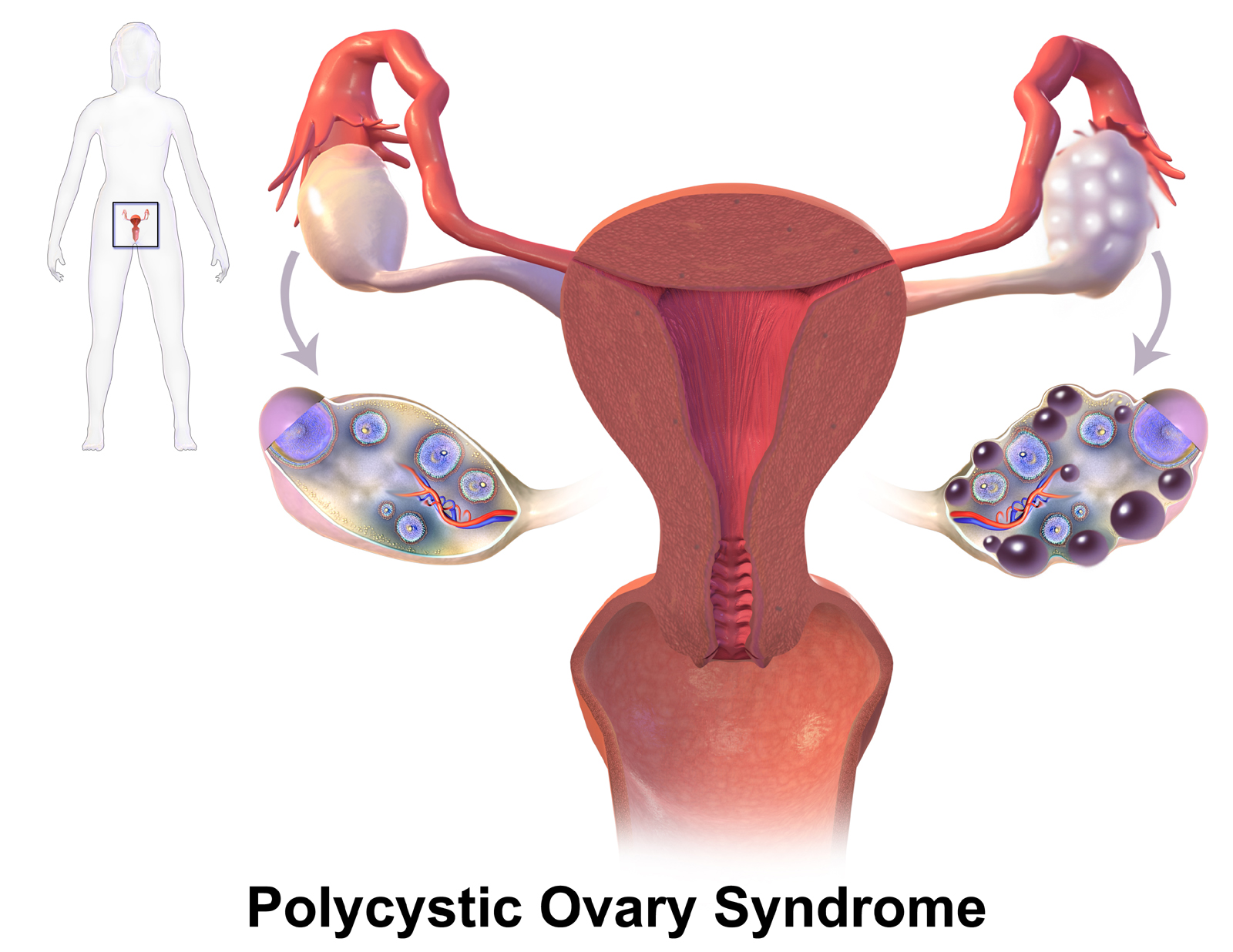
Metformin works by improving insulin sensitivity and lowering insulin levels, which can potentially help restore regular ovulation and reduce androgen (male hormone) levels. Glimepiride, by boosting the body's own insulin secretion, may further help balance metabolic markers when Metformin alone isn't enough.
This combination can:
- Improve menstrual regularity and ovulatory frequency.
- Potentially reduce serum testosterone and hirsutism (excess hair growth) scores.
- It is often used alongside clomiphene or letrozole in fertility treatments.
Adjunct in Weight Management for Insulin-Resistant Patients
For individuals with obesity and insulin resistance, the combination of Metformin and Glimepiride can be beneficial. Metformin's ability to regulate insulin, paired with Glimepiride, helps stabilize blood sugar without significantly increasing body weight – a key concern for many. This approach is particularly useful for those facing metabolic challenges like impaired glucose processing and excess belly fat. These individuals often experience slower glucose metabolism and high fasting insulin levels.
This treatment offers an additional way to support lifestyle changes and weight-loss medications. However, careful monitoring of blood sugar levels is crucial to prevent low blood sugar, especially in individuals who do not have diabetes.
Pre-Diabetes and Impaired Glucose Tolerance Management
For people experiencing early blood sugar problems like impaired glucose tolerance (IGT) or impaired fasting glucose (IFG), medication can help delay or even prevent the full onset of Type 2 Diabetes Mellitus (T2DM). If Metformin alone isn't enough to lower fasting blood sugar, even though it's typically effective for this, Glimepiride might be added.
This is done cautiously and under specific conditions. The goal is to get blood sugar levels into a healthy range, reduce the damaging effects of high sugar, and protect the pancreas's beta cells. While not common practice, some clinical guidelines do consider giving low doses of Glimepiride to high-risk prediabetic patients with metabolic syndrome.
This approach is particularly relevant for individuals with a family history of diabetes and rising HbA1c levels. However, it's crucial to remember that medication is not a replacement for diet and exercise strategies. Research is still ongoing to fully understand the long-term effects of this intervention.
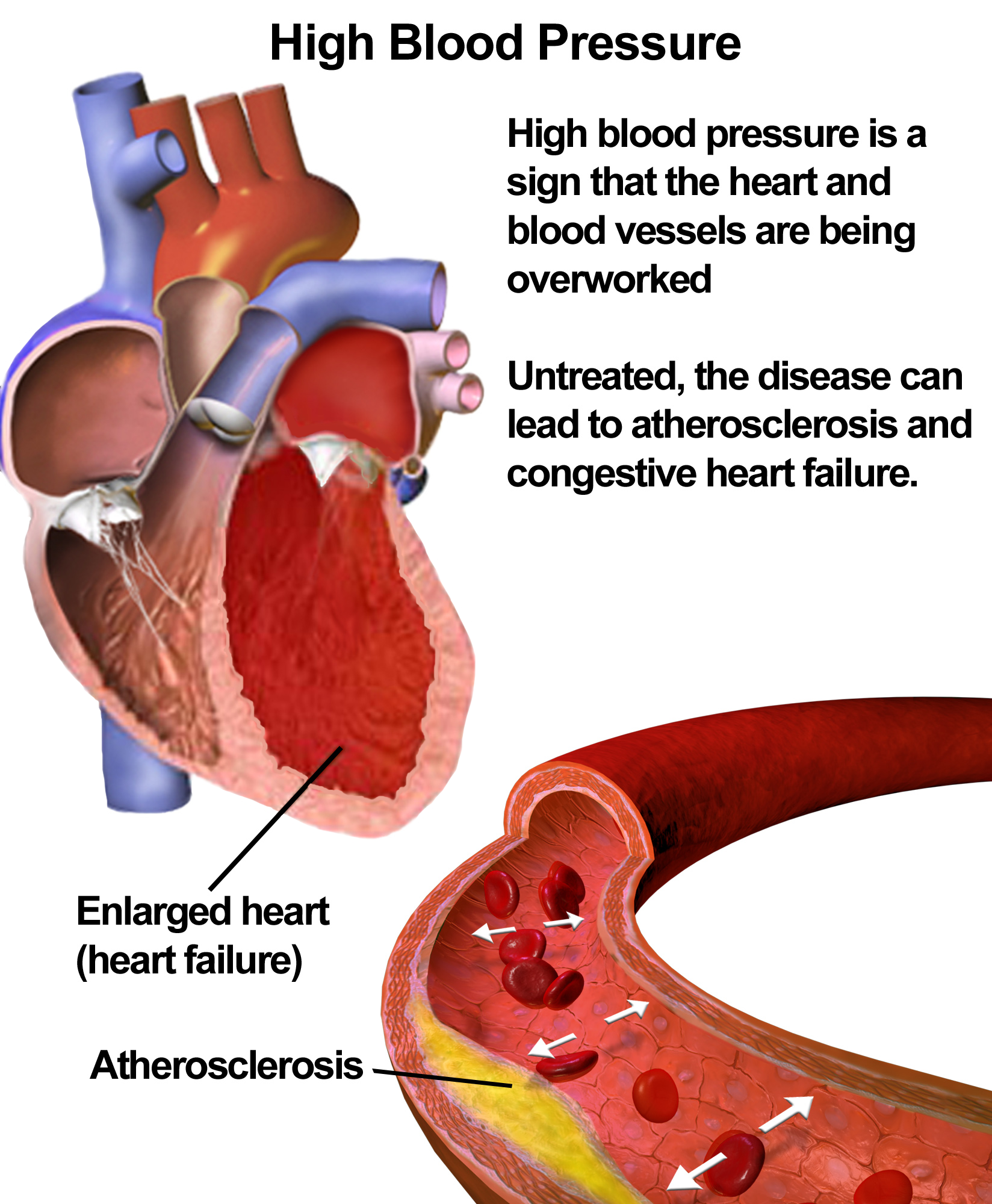
Potential Cardiovascular Protective Effects Under Investigation
While Glimepiride itself might not offer the same direct heart benefits as newer drugs like SGLT2 inhibitors or GLP-1 receptor agonists, recent research suggests that when combined with Metformin, it could provide modest cardiovascular advantages. This is likely due to better blood sugar control, reduced insulin resistance, and improved lipid levels. Metformin is already known to lower the risk of cardiovascular events like heart attacks and strokes in diabetic patients. However, the long-term heart safety of Glimepiride when used alone is still being compared in ongoing studies.
- This combination may offer possible anti-inflammatory effects and help stabilize blood vessel linings.
- In some patient groups, there were improvements in lipid levels and lower blood pressure, pointing to beneficial changes.
Dosage and Administration Guidelines
Standard Dosage Recommendations Based on Patient Profiles
The starting dose of Glador M (Glimepiride/Metformin) depends on a patient's current blood sugar levels, kidney function, and their past experience with diabetes medications. If you're new to this treatment or switching from another regimen, it's important to start cautiously to minimize the risk of digestive upset and low blood sugar.
The initial recommendation is to take 1 mg of Glimepiride along with 500 mg of Metformin daily with breakfast. Doses can then be adjusted based on your blood sugar readings before and after meals.
Titration Strategies for Optimal Glycemic Control
Doses should be increased slowly, usually every one to two weeks. This approach helps prevent stomach upset from Metformin and lowers the risk of low blood sugar from Glimepiride. Don't increase the dose by more than 1 mg of Glimepiride or 500 mg of Metformin at once.
- Blood sugar goals should be personalized based on your HbA1c, age, and other health conditions.
- Increase the dose to the lowest effective amount that helps you reach those goals.
- Frequent self-monitoring of blood glucose (SMBG) is recommended while adjusting your dose.
Timing of Administration with Meals
For digestion and to lower the chances of blood sugar levels, when using Glador M medication, effectively manage your blood sugar levels by taking it with meals. Ideally, with your first main meal of the day. As Metformin benefits, from being taken with food and Glimepiride's insulin boosting effects work well after eating, when glucose levels tend to spike post meal. The morning is the time for taking your daily medication. Please do not bite the extended-release tablets.
Switching from Monotherapy to Combination Therapy
If a patient's blood sugar isn't well-controlled with either Metformin or Glimepiride alone, they can switch to a fixed-dose combination. It's important to find the equivalent dose of their current medication and start the new combination at a similar or even lower dose to minimize side effects.
A doctor should reassess the patient within 7 to 14 days to make sure the dosage is right and that their body is responding well.
- When switching from a high dose of sulfonylurea, watch out for low blood sugar (hypoglycemia).
- Combination pills often make it easier to stick to treatment than taking two separate tablets.
- Always check kidney and liver function before starting the combination therapy.
Missed Dose Management
If you forget a dose of your medication, take it as soon as you remember, unless it's almost time for your next dose. Never double your dose to make up for a missed one, as this can lead to dangerously low blood sugar (from Glimepiride) or a serious condition called lactic acidosis (from Metformin).
- If you miss your morning dose, you can take it later that same day with food.
- If it's nearly time for your next dose, just skip the missed one and continue with your regular schedule.
- It's important to understand the signs of both low blood sugar (hypoglycemia) and high blood sugar (hyperglycemia).

Glimepiride Maximum Dose Per Day
The highest recommended daily dose of Glimepiride is 8 mg. However, taking more than 4 to 6 mg rarely provides extra blood sugar control and can actually increase your risk of low blood sugar. Because of this, doctors often cap the dose at 6 mg for older patients or those with kidney problems.
- The usual dose ranges from 1 to 4 mg per day.
- Never take more than 8 mg per day, no matter what.
- The medication's effectiveness doesn't significantly improve at higher doses.
Common and Serious Side Effects of Glador M
Frequently Reported Side Effects (GI Upset, Dizziness, Headache)
Glador M, which combines Glimepiride and Metformin, is usually well-tolerated. However, some side effects are common, especially when you first start taking it. Digestive issues are the most frequently reported, mainly because of how Metformin works in your gut.
These common side effects include:
- Nausea, diarrhea, and abdominal discomfort: These are usually temporary and often go away within a few days to a couple of weeks.
- Headache and dizziness: You might experience these due to changes in your blood sugar or blood vessel dilation.
- Metallic taste and reduced appetite: These are sometimes noted when taking Metformin.
You can significantly lessen these side effects by gradually increasing your dose and taking the medication with food.
Hypoglycemia: Symptoms, Risk Factors, and Management
Glimepiride, a sulfonylurea medication, can increase the risk of low blood sugar (hypoglycemia), especially in individuals who have kidney problems or inconsistent eating habits. It's crucial to recognize the symptoms, which can range from mild to severe, and require immediate treatment.
Symptoms might include:
- Sweating
- Tremors
- Palpitations

- Confusion
- Blurred vision
- In severe cases, even seizures
Certain factors can raise this risk, such as prolonged fasting, excessive physical activity, consuming alcohol, or taking an overdose.
For treating low blood sugar:
- If conscious, consume 15–20 grams of fast-acting carbohydrates (like glucose tablets or juice).
- If unconscious or severely affected, a glucagon injection might be necessary.
Educating patients thoroughly is vital for early detection and prompt management of these issues.
Lactic Acidosis Associated with Metformin
In rare instances, Metformin can cause a serious condition called lactic acidosis. This happens when too much of the drug builds up in the body, typically in patients with existing kidney problems or low oxygen levels in their tissues. It's characterized by high lactate levels and metabolic acidosis and can have severe, even fatal, consequences if not caught and treated quickly.
Doctors must be very cautious when prescribing Metformin to individuals with risk factors such as:
- Severe heart failure, liver problems, or dehydration.
- Acute illnesses involving oxygen deficiency (like severe lung disease) or serious infections.
Early symptoms often include a general feeling of being unwell, tiredness, muscle pain, difficulty breathing, or unusual sleepiness. If these signs appear, the individual should stop taking Metformin immediately and seek urgent medical help.
Dermatological and Allergic Reactions
Although not common, some people can have allergic reactions to Glimepiride. These might show up as:
- Rashes, itching, or hives
- Sensitivity to sunlight
- In rare cases, severe swelling (angioedema) or a life-threatening anaphylactic reaction
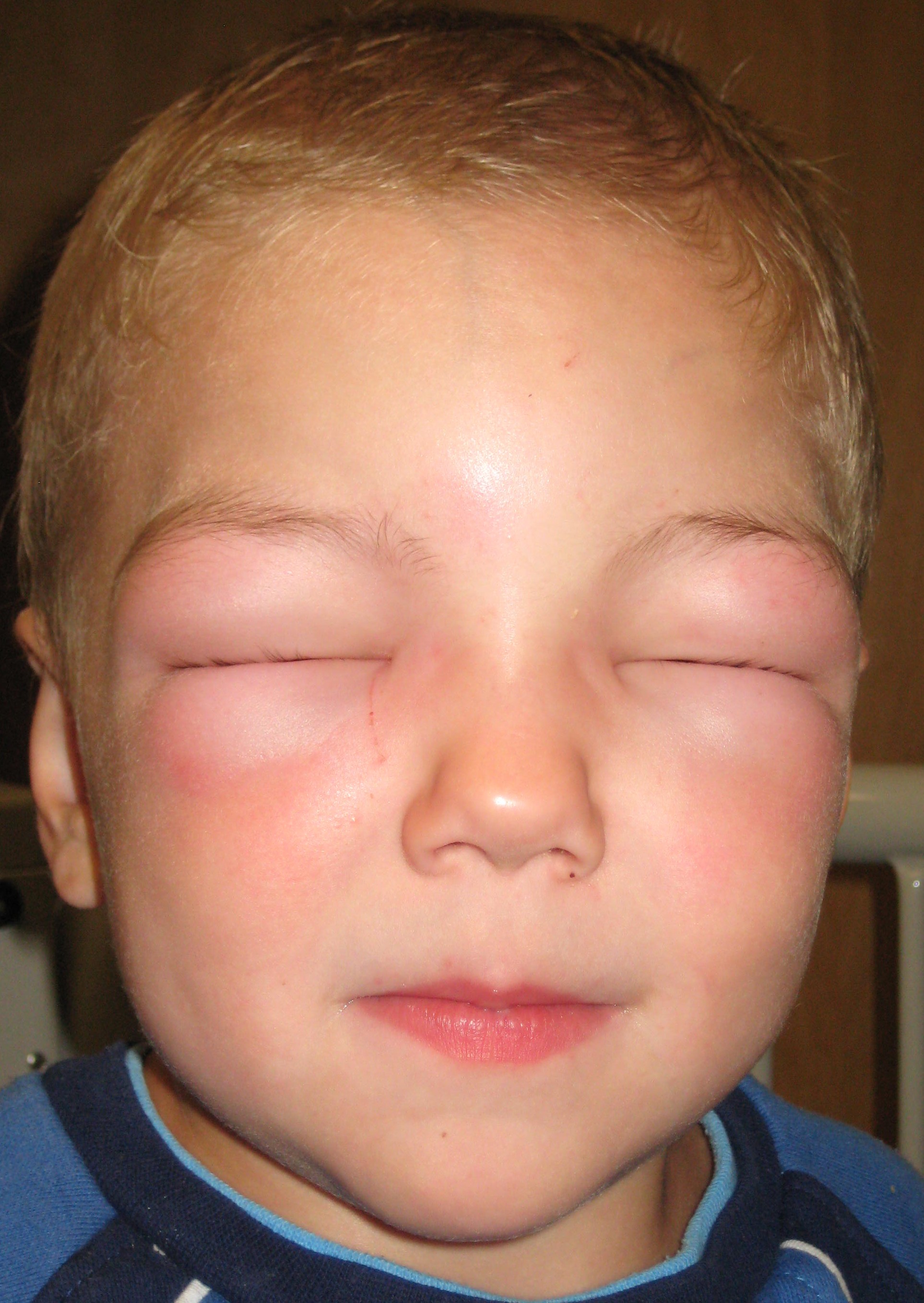
If you experience a moderate to severe allergic reaction, you should stop taking the medication immediately. It's also possible to have a similar reaction to other sulfonylurea drugs.
Glimepiride Side Effects Long-Term
Long-term use of Glimepiride has raised concerns that it might lead to the pancreas's beta cells becoming exhausted, meaning the drug could gradually become less effective at controlling blood sugar over time. Also, constantly stimulating insulin release might contribute to:
- Weight gain and increased body fat.
- Possible cardiovascular risks, although the evidence isn't yet definitive.
- Hypoglycemia (low blood sugar) episodes, which over time might lessen your body's natural warning signs.
Because of these potential issues, it's crucial to regularly re-evaluate treatment to ensure optimal blood sugar control without causing long-term harm to your metabolism.
Glimepiride Weight Loss
Typically, Glimepiride is associated with either maintaining weight or a small weight gain. However, in specific situations—especially when it's combined with Metformin and patients stick to strict dietary rules—you might see a small amount of weight loss. This happens because blood sugar control improves, appetite might decrease, and glucose metabolism becomes more efficient.
Metformin Weight Loss
Metformin often leads to weight loss, in overweight or insulin-resistant individuals by suppressing appetite and improving sensitivity to leptin while also slowing down emptying.
- More noticeably, in individuals with PCOS or those at risk, for developing diabetes before diagnosis.
- Maintaining weight loss usually requires treatment and a commitment to a lifestyle.

Drug Interactions with Glador M
Interaction with Other Antidiabetic Medications
When using Glador M along, with medications that lower glucose levels there is a risk of increasing hypoglycemia or masking changes in blood sugar levels, over time. Its important to be careful and monitor closely when mixing them together.
- Increased risk of hypoglycemia is associated with the use of insulin or GLT receptor agonists.
- DPP hydrolase 5 inhibitors could improve effectiveness without dangers; however medical supervision remains essential.
Effects of Diuretics, Corticosteroids, and Beta-Blockers
Several common medications can affect how Glador M works:
- Diuretics (especially thiazides): These can increase blood sugar by reducing body fluid and making insulin less effective.
- Corticosteroids: These drugs boost sugar production in the liver, which can counteract Metformin's effects.
- Beta-blockers: These can hide the warning signs of low blood sugar, like a fast heartbeat, making it harder to realize you're experiencing hypoglycemia.
Given these interactions, it's crucial to monitor blood sugar frequently and potentially adjust Glador M's dosage when these drugs are used together.
Impact of Alcohol Consumption
Drinking too much alcohol, especially if you have liver problems, while taking Metformin significantly raises the risk of lactic acidosis. Additionally, alcohol can intensify Glimepiride's effect, leading to dangerously low blood sugar.
- This is because alcohol can hinder your body's natural glucose production, increasing the risk of low blood sugar. Long-term heavy drinking can also worsen insulin resistance and unhealthy lipid levels.
- Therefore, it's highly recommended to either completely avoid alcohol or limit it very carefully when on this medication.

Herbal Supplements and Over-the-Counter Drugs
Numerous, over the counter substances could disrupt the way glucose is regulated or how drugs are metabolized.
- St.Johns Wort might change enzyme activity, which can impact drug levels in the body.
- NSAIDs may increase the chance of kidney problems that can impact how Metformin is cleared from the body.
During appointments, it is important for patients to share information about any supplements they are taking to avoid reactions with medications.
Contraindicated Combinations
Some medications and medical situations require you to completely avoid Glador M due to a high risk of serious side effects:
- Iodinated contrast media: These dyes, used in some imaging tests, can significantly increase the risk of lactic acidosis. Because of this, you must stop taking Metformin before and after these procedures.
- Cationic drugs (like cimetidine): These medications can reduce how well your kidneys clear Metformin from your body, potentially leading to its buildup.
- Severe kidney or liver problems: If you have severe issues with your kidneys or liver, Glador M should not be used at all.
Glimepiride Interactions
Glimepiride is processed in your body by an enzyme called CYP2C9. Other medications that either block (inhibit) or speed up (induce) this enzyme can change how well Glimepiride works:
- Inhibitors (like fluconazole) can cause more Glimepiride to stay in your blood, increasing the risk of low blood sugar.
- Inducers (like rifampin) can make Glimepiride less effective at controlling your blood sugar.
Metformin Interactions
Glimepiride is processed in your body by an enzyme called CYP2C9. Other medications that either block (inhibit) or speed up (induce) this enzyme can change how well Glimepiride works:
- Inhibitors (like fluconazole) can cause more Glimepiride to stay in your blood, increasing the risk of low blood sugar.
- Inducers (like rifampin) can make Glimepiride less effective at controlling your blood sugar.
Contraindications for Glador M Use
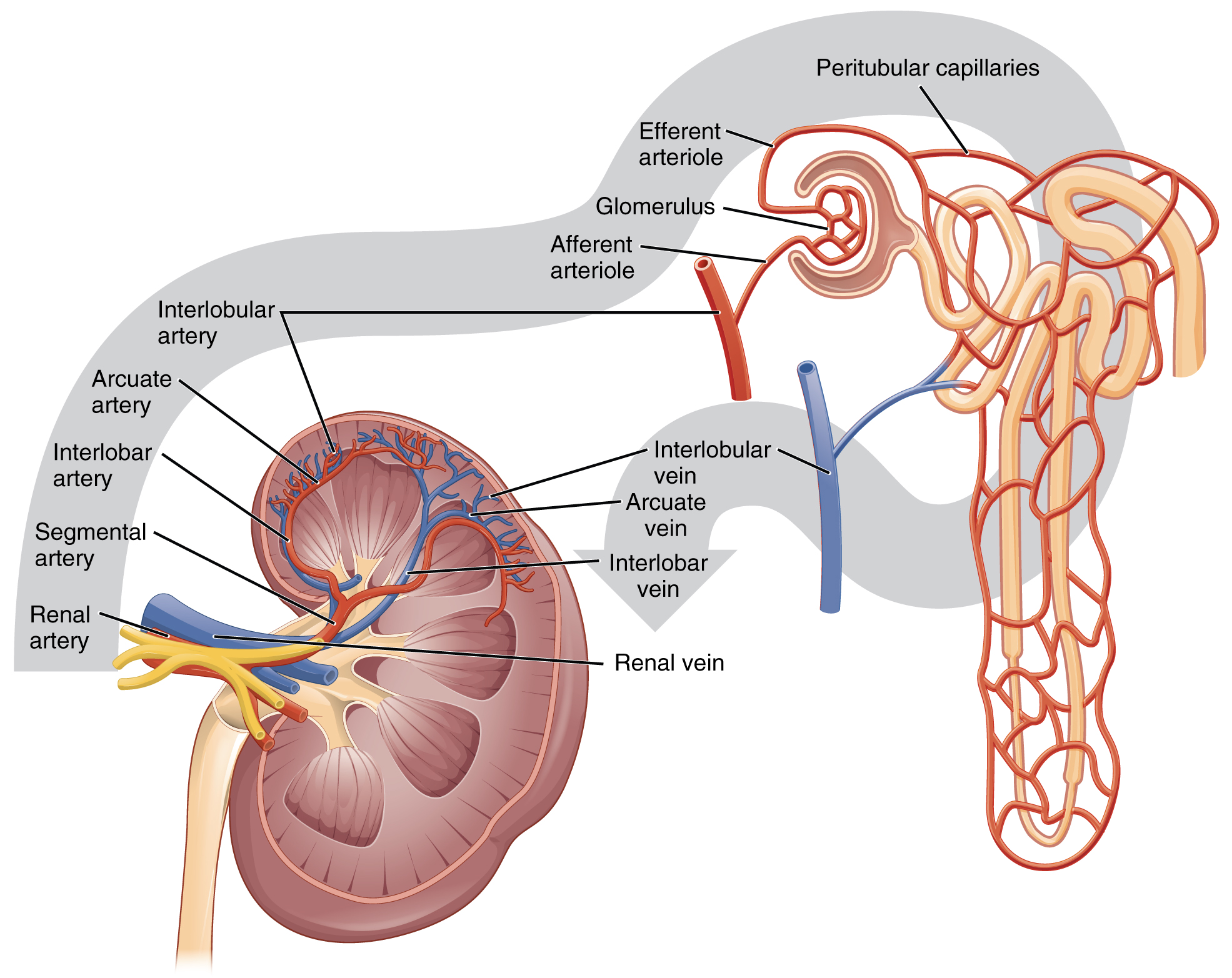
Severe Renal Impairment and eGFR Limitations
Glador M should not be given to people with severe kidney impairment. This is because Metformin, one of its components, is cleared by the kidneys, and severe impairment can cause the drug to build up, leading to a dangerous condition called lactic acidosis. Therefore, a patient's estimated glomerular filtration rate (eGFR) is a critical factor when deciding whether to start or continue this medication.
Regularly checking kidney function is extremely important, especially in older adults or those with fluid imbalances.
Hypersensitivity to Sulfonylureas or Metformin
Glador M must not be given to patients who have a known allergy to Glimepiride, other sulfonylureas, or Metformin. Allergic reactions can range from mild skin rashes to life-threatening anaphylaxis.
It's important to know that if you're allergic to one sulfonylurea, you might also be allergic to others. If you experience any allergic reactions like a rash, hives, or swelling of the face (angioedema), stop taking the medication immediately.
Acute Metabolic Acidosis, Including Diabetic Ketoacidosis
Glador M should not be used if you have acute metabolic acidosis, like diabetic ketoacidosis (DKA) or lactic acidosis. Using it in these situations could make your condition worse and slow down your recovery. Instead, insulin treatment is recommended to restore your body's metabolic balance. You should only restart Glador M once all your metabolic levels are back to normal and stable.
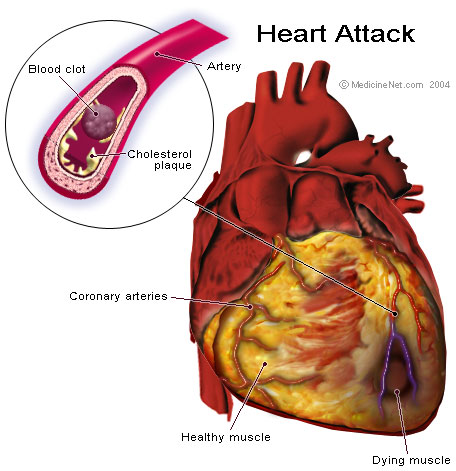
Cardiovascular Instability and Recent Myocardial Infarction
Patients who have recently had a heart attack or are experiencing shock or sudden heart failure are at a greater risk of their tissues not getting enough oxygen. This lack of oxygen is a known trigger for lactic acidosis related to Metformin, according to medical guidelines.
- Therefore, if a patient has these conditions, it's best to wait until their heart condition stabilizes clinically before starting or continuing Glador M.
- Delay starting treatment until heart function returns to normal.
- During acute heart problems, individuals might need to explore alternative treatment options for their diabetes.
Metformin Contraindications
Beyond kidney problems, Metformin should also be avoided in specific situations:
- Severe liver damage significantly reduces your body's ability to clear lactate, increasing the risk of lactic acidosis.
- Alcoholism can both increase lactate production and impair liver function, further raising the risk of acidosis.
- Radiological tests using iodinated contrast agents can potentially cause a temporary decline in kidney function, which can lead to Metformin buildup and acidosis.
It's strongly advised to pause Metformin during acute illnesses and before contrast imaging studies.
Warnings and Important Precautions
Risk of Lactic Acidosis: Signs and Emergency Protocols
Lactic acidosis is a rare but life-threatening medical emergency. It's crucial to identify it quickly and stop Metformin immediately if it's suspected. The risk of this condition increases if you have kidney problems, low oxygen in your tissues, dehydration, or liver disease.
Watch out for these signs:
- Rapid breathing (Kussmaul respiration)
- Muscle weakness, abdominal pain, or low blood pressure
- Confusion, drowsiness, and in severe cases, coma
If lactic acidosis is suspected, you need to be hospitalized right away for supportive care. Doctors may also consider hemodialysis to remove Metformin from your body.
Monitoring of Renal and Hepatic Function
It's essential to regularly monitor kidney function, especially for patients with existing kidney issues or those taking medications that could harm the kidneys. Similarly, liver function should be assessed before starting treatment and periodically thereafter.
Key monitoring includes:
- Kidney function tests, such as checking serum creatinine levels and estimated glomerular filtration rate (eGFR), ideally every 3 to 5 months.
- Liver enzymes like ALT and AST are used to detect potential liver damage.
- Treatment should not be given if a patient has acute kidney failure or active liver dysfunction.
Avoidance of Alcohol and Dehydration
Consuming alcohol can increase the chances of developing lactic acidosis and worsen the risk of low blood sugar levels when taking Glimepiride specifically. Dehydration caused by vomiting or diarrhea as strenuous exercise, can lower kidney function and amplify potential health hazards.
- Alcohol consumption is best limited or abstained from altogether.
- It's important to stay properly hydrated during times of illness with a fever.
Taking a break during periods of dehydration is usually necessary to avoid issues that may arise.
Increased Sun Sensitivity and Skin Reaction Precautions
Glimepiride belongs to a class of medications known as sulfonylureas. Has the potential to make your skin more sensitive to sunlight exposure, which can lead to sunburn or skin rashes.
- I suggest using sunscreen and wearing clothing.
- Please stop taking the medication if you experience photosensitive dermatitis.
Skin issues that show up on your skin should be checked by a doctor to see if you need to visit a dermatologist for evaluation.

Periodic HbA1c and Fasting Glucose Monitoring
Consistently monitoring blood sugar levels is essential for managing your treatment and preventing complications. It allows you to adjust medication doses as needed and quickly spot when your current treatment plan isn't working effectively.
- You should have your HbA1c levels checked every three months until they stabilize. Once stable, you can reduce this to twice a year.
- For individuals at risk, blood sugar monitoring schedules may vary.
Any adjustments to your therapy should be tailored to your specific blood sugar patterns and overall clinical situation.
Careful Administration and Monitoring Recommendations
Patients with Mild-to-Moderate Renal Impairment
For individuals with kidney problems that affect their ability to filter waste, the way Metformin is processed in the body can change, as it's primarily removed by the kidneys. While Glador M should be avoided in severe kidney dysfunction, patients with mild to moderate impairment (eGFR 45–60 mL/min per 1.73 mg) might still be prescribed it, but they would require very close monitoring during treatment.
- If kidney function worsens, consider reducing the dosage or switching to alternative medications.
- Exercise caution to prevent lactic acidosis when dealing with dehydration or sudden illness.

Concomitant Use with Other Hypoglycemic Agents
When Glador M is used with insulin or other medications like meglitinides or additional sulfonylureas—all of which can increase the risk of low blood sugar (hypoglycemia)—it's vital to carefully adjust dosages and closely monitor glucose levels.
To manage these combinations safely:
- Start with small amounts when blending medications to prevent sharp drops in glucose.
- Adjust insulin schedules as needed to minimize overlapping effects.
- Educate patients on how to recognize and treat hypoglycemia themselves.
For these dual and triple therapies to be effective, following structured titration protocols and having regular outpatient follow-ups are essential.
Initiation in Elderly or Frail Patients
When considering Glador M for elderly or frail individuals, it's important to be cautious. Their kidney function naturally declines with age, and their bodies may react differently to medications, increasing the risk of side effects.
- Always start with the lowest possible dose and only increase it if absolutely necessary.
- It's crucial to balance the goal of controlling blood sugar with ensuring their safety and quality of life.
Additionally, for this group, it's vital to review all medications they're taking (medication reconciliation) and assess their risk of falls.
Lifestyle and Dietary Adherence Importance
How well Glador M works is greatly impacted by how consistently patients stick to their lifestyle changes. The medication is most effective when combined with regular meal times, structured physical activity, and disciplined nutrition.
- Skipping meals or eating irregularly can lead to low blood sugar (hypoglycemia) due to Glimepiride.
- Weight loss and improved insulin sensitivity make Metformin work even better.
Patient education should focus on encouraging long-term behavioral changes. Healthcare providers need to stress the importance of personalized diet plans and consistent participation in physical activity.
Use in Special Populations
Administration to Elderly Patients
Dose Adjustment Due to Renal Clearance Changes
In individuals careful adjustment of Glimepiride and Metformin doses is crucial, due to the decline in kidney function associated with aging. As renal filtration decreases the concentration of these drugs, in the body rises, with Metformin raising the chance of acidosis occurring.
- Regularly calculating e GFR is essential, than relying on serum creatinine levels.
- It is advised to restrict the dosage of Glimepiride to no more, than 4 mg, per day for patients aged 65 and above.
Risk of Hypoglycemia and Falls
In individuals, hypoglycemia can show up in ways and is a major factor in causing falls, broken bones, and hospital stays. Glimepiride's extended effects can lead to blood sugar levels in this group.
- Symptoms might manifest as confusion or dizziness, with speech difficulty of showing indicators.
- Nighttime low blood sugar levels might be overlooked. They can result in a decrease in functioning.

Monitoring and Caregiver Instructions
Education for caregivers is crucial in observing symptoms of blood sugar and ensuring consistent medication usage is maintained.The routine assessment of abilities along, with monitoring nutrition and hydration levels are aspects to consider carefully.
- Encouraging the utilization of pill organizers. Keeping track of medication usage.
- Encourage those providing care to identify shifts in behavior promptly and respond appropriately.
Glimepiride Side Effects in Elderly
In individuals who take Glimepiride for a period of time might face a higher risk of experiencing low blood sugar levels or gaining weight and even encountering cardiovascular strain as potential side effects to Carefully if aiming for strict blood sugar control may not be the best approach, in certain cases.
Administration During Pregnancy and Lactation
Risk Category and Evidence from Animal/Human Studies
Metformin falls under pregnancy category B. Has been backed by human studies indicating its safety during gestational diabetes cases specifically. On the other hand Glimepiride is categorized as class C for pregnancy with data available and some observed teratogenic effects, in animal studies.
- Metformin is sometimes prescribed during pregnancy with the guidance of a specialist.
- It's usually best to steer clear of using Glimepiride due to its effects on the fetus

Recommendations During Pregnancy Planning
Women who are considering getting pregnant should switch from Glador M to either insulin or Metformin as a therapy while being monitored by their obstetrician. Receiving counseling before conception helps in planning treatment and reduces any harm to the unborn child.
- The use of acid supplements should begin at this time.
- Prior to becoming pregnant it is important to ensure that your HbA1c levels are well managed.
Lactation Safety of Glimepiride and Metformin
Metformin is released into breast milk in quantities. It is deemed safe for breastfeeding mothers to use it while nursing their babies. The safety of Glimepiride during breastfeeding is uncertain as there is research on its transfer into breast milk.
- Metformin is the preferred choice for postpartum treatments.
- Monitor babies for any signs of blood sugar or stomach issues.

Alternative Therapy Considerations
Insulin continues to be the preferred choice for managing diabetes during pregnancy and breastfeeding due to its documented safety record. For women who have difficulties with insulin tolerance, Metformin could be considered as a solution, with medical supervision.
Pediatric Use and Administration to Children
Approved Age Ranges for Use
Metformin has been given the light by the FDA for kids who are 10 years old and up and dealing with type 2 diabetes; on the flip side, though Glimepiride doesn't have as much backing, for use, in children, and there hasn't been a thorough review of combining it with Glador M specifically for kids.
Limited Data and Clinical Study Outcomes
There is a lack of long-term trials studying the effects of Glimepiride in children and adolescents under 18 years old. Although certain studies suggest its effectiveness, in this population group, to some extent, the safety signals associated with its use are not sufficiently understood. As a result of this data, it is difficult to recommend its use for individuals under 18 years old.
Risk-Benefit Analysis in Adolescent Patients
For teenagers with insulin resistance who aren't responding well to Metformin alone, Glimepiride might be considered cautiously. This decision should be made by an endocrinologist on a case-by-case basis, carefully weighing the potential benefits of improved blood sugar control against the risks of low blood sugar (hypoglycemia), weight gain, and challenges with treatment adherence.
- Off-label use of Glimepiride should only be reserved for difficult-to-treat cases.
- Providing psychosocial support and clear guidance is crucial to help teenagers stick to their treatment plan.
Overdose and Emergency Management
Symptoms of Metformin and Glimepiride Overdose
Overdosing on Glador M (a combination of Metformin and Glimepiride) can have life-threatening consequences, as each drug carries its own risks:
- Too much Metformin can cause lactic acidosis, with symptoms like nausea, stomach pain, deep, rapid breathing (Kussmaul respiration), confusion, and eventually heart failure.
- An overdose of Glimepiride can lead to dangerously low blood sugar (hypoglycemia), resulting in heavy sweating, uncontrollable shaking, loss of consciousness, seizures, or even a coma.
Combining these drugs in an overdose significantly destabilizes the body and requires immediate medical attention.

Management of Severe Hypoglycemia
Severe low blood sugar (hypoglycemia) caused by Glimepiride is a medical emergency that needs immediate treatment to prevent brain damage. Here's what to do:
- For a conscious patient, give 15 to 20 grams of sugar immediately, such as oral glucose gel or juice.
- If the patient is unconscious or unable to swallow, administer IV dextrose (50%) or a glucagon injection.
- In some severe cases, continuous dextrose infusion and heart monitoring might be necessary.
Be aware that low blood sugar can return for 24 to 48 hours after an overdose, as Glimepiride has long-lasting effects.
Treatment Protocols for Lactic Acidosis
Lactic acidosis caused by Metformin is a serious medical emergency that needs quick recognition and aggressive treatment to prevent organ failure. The core of treatment involves:
- Administering intravenous sodium bicarbonate to correct the metabolic acidosis.
- Providing supportive care, which includes oxygen and fluid replenishment.
This diagnosis is confirmed by blood tests showing a low pH, a high anion gap, and elevated serum lactate levels (above 5 mmol/L). The top priority in these cases is always patient stabilization.
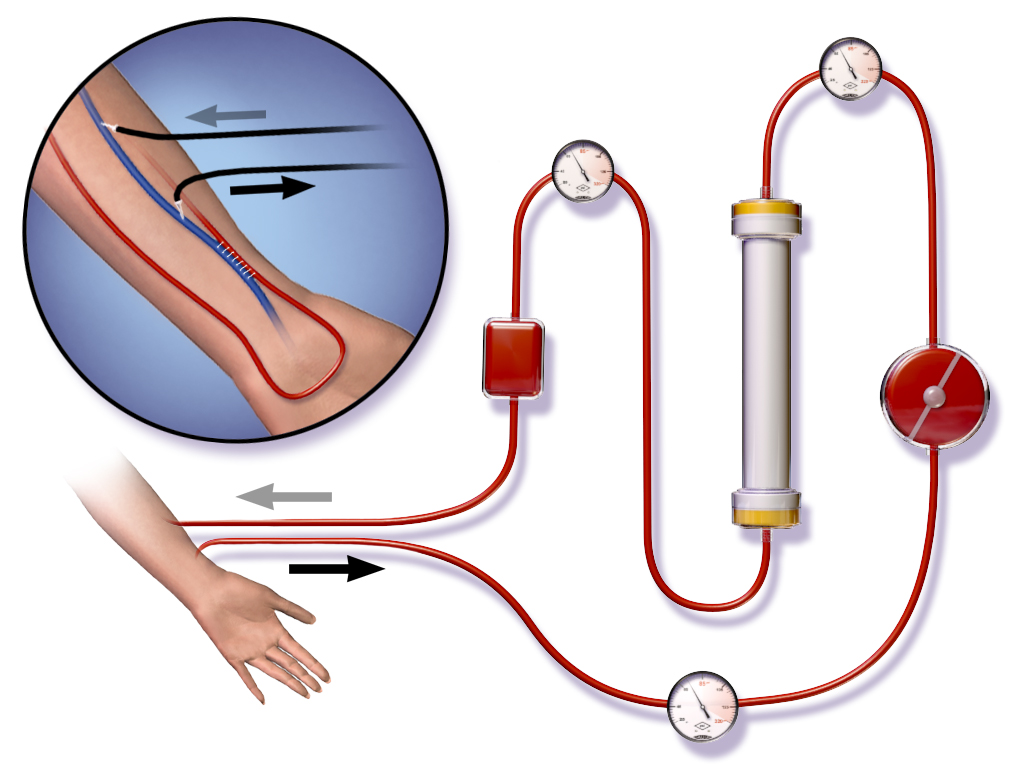
Emergency Supportive Care and Dialysis Considerations
When facing severe and prolonged low blood sugar from Glimepiride or Metformin toxicity, hemodialysis is a crucial treatment.
- Hemodialysis effectively removes accumulated Metformin from the body and efficiently corrects acidosis. In cases of Glimepiride overdose combined with kidney failure, dialysis might also be needed to help eliminate the drug. For patients who are unstable, Continuous Renal Replacement Therapy (CRRT) might be necessary.
- Patients with these conditions are typically admitted to Intensive Care Units (ICUs), where their organ function and metabolic levels are continuously monitored.
Handling and Storage Instructions
Recommended Storage Conditions for Stability
To ensure Glador M tablets remain effective, they must be stored properly:
- Keep them at a temperature ideally between 68°F to 77°F (20°C to 25°C). Minor fluctuations, from 59°F to 86°F (15°C to 30°C), are also acceptable.
- Store them away from areas with humidity above 60% to prevent damage.
- Storing medications incorrectly can reduce their effectiveness and jeopardize their ability to provide the intended health benefits and safety.
Protecting from Moisture, Heat, and Light
Exposure to stressors in the environment speeds up the breakdown of substances, leading to their deterioration quickly than usual measures are taken to avoid this situation;
- Avoid exposing it to direct sunlight or excessive heat sources.
- Avoid keeping items in places like bathrooms.
- Blister packs should be kept closed until they're ready to be used to avoid absorbing moisture.
Shelf Life and Disposal Guidelines
Glador M typically remains effective for 2 to 3 years from its manufacturing date, depending on its packaging and how it's stored. Patients and caregivers should keep these important points in mind:
- Always check the expiration dates on the packaging.
- Dispose of any unused medication through designated return programs.
- Never flush medications down the toilet unless you're specifically instructed to do so.
Pharmacists are key in guiding individuals on proper medication disposal methods to help protect the environment.
Handling Precautions for Caregivers and Pharmacists
Healthcare providers administering Glador M must follow strict hygiene protocols:
- Wash hands thoroughly before and after handling the tablets.
- Do not break or cut the tablets unless specifically instructed to do so.
- If you are giving the medication to someone with a compromised immune system, remember to wear gloves.
Pharmacists are responsible for ensuring accurate labeling, adhering to batch tracking, and meeting storage requirements when dispensing the medication.
Considerations
Importance of Regular Follow-Up and Lab Testing
To ensure your treatment is effective and to catch any potential problems early, regular medical check-ups are essential. These appointments allow for necessary adjustments to your medication dosage.
Specifically, you should have:
- Serum creatinine levels and estimated glomerular filtration rate (eGFR) checked twice a year to assess kidney function.
- Periodic checks of liver enzymes (like ALT and AST) to identify any liver issues.
- Additionally, regular foot and eye exams are recommended to detect any diabetes-related complications early on.
Patient Counseling and Education
When people are well-informed about their condition, they're more likely to stick to their treatment plans and spot early signs of trouble. Key educational points to emphasize include:
The importance of consistent meal timings to prevent significant fluctuations in blood sugar.
- Understanding the symptoms of acidosis and knowing when to get immediate medical help.
- Avoiding alcohol and medications that can interact negatively with their treatment.
- Written materials and online resources can be very helpful additions to in-person counseling sessions.
Re-evaluation of Therapy Effectiveness Over Time
Diabetes is a progressive condition, so it's crucial to regularly review treatment plans to ensure they remain effective.
Adjustments may be needed due to:
- Changes in body weight, variations in kidney function, or new health conditions.
- The introduction of other medications could affect how your body processes glucose.
- Ultimately, treatment plans must evolve over time to effectively match a patient's changing health needs.
Glador M, Glimepiride/ Metformin FAQ
- What is Glimepiride used for?
- Can I take Glimepiride at night?
- Does Glimepiride cause weight gain?
- What is Glimepiride?
- How long does Glimepiride stay in your system?
- Does Glimepiride cause diarrhea?
- Does Glimepiride cause weight loss?
- Which is safer, Metformin or Glimepiride?
- Does Glimepiride cause hair loss?
- How long does it take Glimepiride to work?
- Can I take Jardiance and Glimepiride together?
- Can Glimepiride cause weight gain?
- Can you take Glimepiride and Metformin together?
- Can you take Glipizide and Glimepiride together?
- How fast does Glimepiride work?
- Is Glimepiride safe?
- How long does Glimepiride take to work?
- Can I take Glimepiride twice a day?
- Which is better, Glimepiride or Glipizide?
- Difference between Glipizide and Glimepiride?
- When to take Glimepiride?
- Are Glimepiride and Glipizide the same?
- Are Glimepiride and Metformin the same?
- Are Glimepiride and Glipizide the same thing?
- What are Glimepiride used for?
- What are Glimepiride tablets used for?
- Can Glimepiride cause diarrhea?
- Can Glimepiride cause hypoglycemia?
- Can Glimepiride be taken twice a day?
- Can Glimepiride cause weight gain?
- Can Glimepiride cause weight gain?
- Can Glimepiride and Vildagliptin be taken together?
- Can Glimepiride and Metformin be taken together?
- How Glimepiride works?
- Glimepiride how to take?
- Glimepiride how many times a day?
- Glimepiride how long does it take to work?
- Glimepiride how long does it take to work?
- What Glimepiride used for?
- Glimepiride what does it do?
- When Glimepiride stops working?
- When Glimepiride should be taken?
- Glimepiride when to eat?
- Glimepiride when to stop before surgery?
- Glimepiride when to use?
- Glimepiride when to give?
- Where does Glimepiride metabolized?
- Where is Glimepiride manufactured?
- Where is Glimepiride made?
- Where is Glimepiride metabolized?
- Glimepiride which class of drug?
- Why Glimepiride is taken before food?
- Why Glimepiride is used with metformin?
- Why Glimepiride is better than Gliclazide?
- Why Glimepiride cause hypoglycemia?
- Why is Glimepiride a high risk medication?
- Will Glimepiride cause weight gain?
- Will Glimepiride lower blood sugar?
- Will Glimepiride cause weight loss?
- Will Glimepiride cause diarrhea?
- Will Glimepiride raise blood pressure?
- Will Glimepiride cause hair loss?
- Does Metformin cause weight loss?
- How to lose weight fast on Metformin?
- Signs Metformin is working?
- Does Metformin help with weight loss?
- Does Metformin cause diarrhea?
- Best time to take Metformin?
- Foods to avoid while taking Metformin?
- How long does it take for Metformin to work?
- How does Metformin help you lose weight?
- Why does Metformin cause diarrhea?
- Does Metformin help you lose weight?
- What is the lowest dose of Metformin you can take?
- How long does Metformin take to work?
- Benefits of Metformin?
- Does Metformin make you sleepy?
- When is the best time to take Metformin?
- Metformin dosage for weight loss in non diabetics?
- Does Metformin cause weight gain?
- How long does Metformin stay in your system?
- How long does it take Metformin to work?
- How to take Metformin?
- What happens if you take too much Metformin in one day?
- Best time to take Metformin for weight loss?
- What is the lowest dose of Metformin you can take for PCOS?
- Can Metformin cause diarrhea?
- What is Metformin used for other than diabetes?
- Can I stop taking Metformin when my sugar back to normal?
- How fast does Metformin work?
- Does Metformin cause constipation?
- Alternative to Metformin?
- How does Metformin work for weight loss?
- Can you take Metformin and Ozempic together?
- Metformin constipation?
- How long for Metformin to work?
- How to stop Metformin diarrhea?
- Best time of day to take Metformin?
- Can you take Metformin while pregnant?
- Can Metformin cause weight gain?
- What happens if you take Metformin and don't need it?
- Can you take berberine with Metformin?
- Can you drink on Metformin?
- Can Metformin cause constipation?
- Can Metformin cause Fatigue?
- Does Metformin cause kidney damage?
- Are Metformin bad for you?
- Are Metformin side effects temporary?
- Are Metformin and Ozempic the same?
- Are Metformin and Ozempic similar?
- Are Metformin and Berberine the same?
- Can Metformin help with weight loss?
- Can Metformin be taken without food?
- Can Metformin cause hypoglycemia?
- Can Metformin cause itchy skin?
- Can Metformin cause kidney damage?
- How metformin cause lactic acidosis?
- How Metformin helps in weight loss?
- How Metformin causes vitamin B12 deficiency?
- What Metformin does to the body?
- When Metformin should be taken?
- When Metformin is contraindicated?
What is Glimepiride used for?
Glimepiride is prescribed for controlling type 2 diabetes, assisting in reducing blood sugar levels through encouraging insulin release from the pancreas beta cells as part of a regimen that includes adjustments and physical activity, or in conjunction with other antidiabetic drugs.
Can I take Glimepiride at night?
Glimepiride is typically ingested in the morning either with or just before the meal of the day, as taking it at night is discouraged to avoid potential nighttime low blood sugar levels caused by its stimulation of insulin production.
Does Glimepiride cause weight gain?
Glimepiride can lead to weight gain in individuals, as it may boost insulin secretion and enhance glucose utilization, which could potentially result in weight gain if calorie intake is not monitored effectively.
What is Glimepiride?
Glimepiride functions as a medication belonging to the sulfonylurea class category, which enhances the secretion of insulin from beta cells in the pancreas to reduce blood sugar levels in individuals with type 2 diabetes.
How long does Glimepiride stay in your system?
The time it takes for Glimepiride to be reduced by half in the body is around 5 to 8 hours; however, its ability to lower glucose levels can continue for up to 24 hours before leaving the system, which may vary from 1– 2 days based on kidney and liver functions.
Does Glimepiride cause diarrhea?
Diarrhea is not a reaction of Glimepiride; however it might manifest in certain cases. Should this symptom persist or become severe, it's advisable to inform a professional, as it could signal intolerance or an underlying condition.
Does Glimepiride cause weight loss?
Glimepiride usually does not lead to weight loss. Rather may result in weight gain instead. It is advisable to assess any weight loss that does happen to exclude factors or possible negative impacts.
Which is safer, Metformin or Glimepiride?
Metformin is usually seen as safer compared to Glimepiride when it comes to the chances of hypoglycemia and cardiovascular issues as Glimepiride poses a risk of hypoglycemia and weight gain; however, Metformin has a positive safety record, with fewer side effects.
Does Glimepiride cause hair loss?
Hair loss is not commonly reported as an effect of Glimepiride; however if you experience thinning of hair, it is advisable to consult with a healthcare professional as it could be linked to fluctuating blood sugar levels or other medications you are taking or any underlying health issues you may have.
How long does it take Glimepiride to work?
Glimepiride usually starts reducing blood sugar levels within 2 to 3 hours of taking it by mouth. However, the best results are observed after using it for a days to a few weeks, depending on how your body responds.
Can I take Jardiance and Glimepiride together?
Glimepiride and Jardiance (Empagliflozin) can be taken concurrently under the care of a healthcare professional. This pairing might improve blood sugar management. Also raises the chance of blood sugar levels, particularly when dietary habits are erratic.
Can Glimepiride cause weight gain?
Weight gain is indeed listed as a known side effect of Glimepiride medication due to its ability to release insulin and potentially lead to the storage of fat when calorie consumption surpasses energy expenditure.
Can you take Glimepiride and Metformin together?
Glimepiride and Metformin are commonly recommended in combination to enhance management efforts. Glimepiride encourages insulin production while Metformin works to lessen liver glucose output and enhance insulin receptivity.
Can you take Glipizide and Glimepiride together?
Combining Glipizide and Glimepiride is usually not advised because both are sulfonylureas with functionalities that can elevate the chance of hypoglycemia without providing any advantages.
How fast does Glimepiride work?
Glimepiride typically begins to reduce blood sugar levels within 2 to 3 hours after taking it and shows its effects, around 2 to 4 hours later. It's common to notice improvements in your condition within a day of starting the treatment.
Is Glimepiride safe?
Glimepiride is generally seen as safe for individuals with type 2 diabetes when used correctly; however, it is important to keep an eye out for blood sugar levels potential weight gain, and any possible interactions with medications.
How long does Glimepiride take to work?
Glimepiride starts working after being taken into the body. Shows its maximum effect in lowering glucose levels within 2 to 4 hours of consumption.Regular use over a period of days to weeks results in the control of blood sugar levels.
Can I take Glimepiride twice a day?
Glimepiride is usually taken once a day as directed by a doctor; In situations where blood sugar management's not ideal, a healthcare provider might suggest splitting the dosage into multiple times per day. Remember, it's best to avoid adjusting your medication without consulting a healthcare professional.
Which is better, Glimepiride or Glipizide?
Sulfonylureas are both used to treat type 2 diabetes; however Glimepiride has a period of effectiveness and might have a slightly reduced chance of hypoglycemia associated with it compared to others, in its class. The decision is usually based upon how each individual responds to the medication and their accompanying medical conditions.
Difference between Glipizide and Glimepiride?
Glipizide has a life and is commonly chosen for older individuals or those with a higher likelihood of experiencing low blood sugar levels while Glimepiride provides an extended period of effectiveness and may require less frequent dosages.
When to take Glimepiride?
Glimepiride is recommended to be taken a day either with or right before your meal of the day in order to lower the chances of experiencing low blood sugar levels and maximize its effectiveness.
Are Glimepiride and Glipizide the same?
While both Glimepiride and Glipizide belong to the sulfonyurea class of drugs they vary in their strength how long they last in the body and how they are processed by the body. It's essential to seek advice before switching between these medications.
Are Glimepiride and Metformin the same?
Glimepiride functions as a sulfonylurea that boosts insulin release; meanwhile Metformin lowers glucose output. Enhances insulin sensitivity. They operate in ways that are frequently prescribed together.
Are Glimepiride and Glipizide the same thing?
Glimepiride and Glipizide belong to medications in the sulfonylureas category with variations in dosages, effectiveness, and duration of impact.
What are Glimepiride used for?
Glimepiride is commonly prescribed to manage blood sugar levels in individuals with type 2 diabetes when diet and exercise, along with Metformin do not provide control.
What are Glimepiride tablets used for?
Glimepiride tablets are commonly recommended for controlling type 2 diabetes by triggering insulin release from the pancreas to lower blood sugar levels.
Can Glimepiride cause diarrhea?
Experiencing diarrhea as a side effect of Glimepiride is rare; if this issue arises it could be linked to sensitivity or interactions with other medications and ought to be communicated to a medical professional.
Can Glimepiride cause hypoglycemia?
Glimepiride has the potential to lead to blood sugar levels known as hypoglycemia when meals are missed or when taken alongside medications that lower glucose levels; hence it's crucial to monitor blood sugar levels consistently while undergoing treatment.
Can Glimepiride be taken twice a day?
Glimepiride is typically prescribed for intake; however, in certain cases, splitting the dosage may be recommended, but it is important to do so under medical guidance to reduce the risk of low blood sugar levels.
Can Glimepiride cause weight gain?
Glimepiride can cause weight gain when taken with a high-calorie diet or lack of activity since it boosts insulin levels that encourage storing fat.
Can Glimepiride cause weight gain?
Glimepiride has been found to contribute to weight gain in individuals who may experience this effect, particularly when they attain control through consuming more calories than necessary.
Can Glimepiride and Vildagliptin be taken together?
Glimepiride and Vildagliptin can be administered together safely as they work in tandem to improve glucose regulation; however, close supervision is necessary to watch for blood sugar levels.
Can Glimepiride and Metformin be taken together?
It's quite common for doctors to recommend taking them when treating type 2 diabetes. Metformin helps your body respond better to insulin and Glimepiride helps your body produce insulin well; this combination works together to lower blood sugar levels effectively.
How Glimepiride works?
Glimepiride encourages the pancreas beta cells to release insulin by shutting down ATP potassium channels This process results in membrane depolarization and the influx of calcium leading to the secretion of insulin.
Glimepiride how to take?
Its recommended to take Glimepiride a day either with or right, before your meal of the day to reduce the chance of experiencing low blood sugar levels.
Glimepiride how many times a day?
Glimepiride is usually consumed once a day, as part of the medication routine, for an individuals wellbeing and health management purposes. In customized treatment plans or schedules tailored to the needs and conditions of an individual patient; there could be instances where the prescribed dosage is divided or split into smaller portions throughout the day; however such adjustments should only be made following guidance and oversight from a medical professional or healthcare provider.
Glimepiride how long does it take to work?
Glimepiride begins to take effect in 2 to 3 hours. Shows its impact, around 2 to 4 hours after taking it. Using it regularly results in control of blood sugar levels over a period of days, to weeks.
Glimepiride how long does it take to work?
Glimepiride begins to have an impact, after intake; however, continuous dosing, over time is necessary for optimal blood sugar management benefits to manifest fully.
What Glimepiride used for?
Glimepiride is commonly utilized in the management of type 2 diabetes aiding in reducing blood sugar levels for patients whose diabetes is not effectively managed through diet and exercise alone.
Glimepiride what does it do?
Glimepiride reduces blood sugar levels by boosting insulin release from the pancreas, aiding in managing blood sugar levels in individuals suffering from type 2 diabetes.
When Glimepiride stops working?
Over time Glimepiride might lose its effectiveness as a result of declining beta cell function, leading to what's termed failure, which could necessitate adjustments in treatment strategies.
When Glimepiride should be taken?
It is recommended to take it a day with your meal to lower the chance of low blood sugar and get the most out of it.
Glimepiride when to eat?
It's best to eat after you've taken Glimepiride. Within 15-30 minutes. To reduce the chances of experiencing low blood sugar levels.
Glimepiride when to stop before surgery?
Glimepiride is typically recommended to be stopped on the day of the surgery and potentially earlier depending on the type of surgery and fasting guidelines, in place always ensuring to adhere to your doctor's advice.
Glimepiride when to use?
When your diet and exercise routine coupled with Metformin don't fully manage your type 2 diabetes control needs; incorporating Glimepiride is beneficial to help regulate blood sugar levels consistently by taking it at the same time every day.
Glimepiride when to give?
Administer Glimepiride, before or during your meal of the day, to synchronize its maximum impact with the increase, in glucose levels after eating meals.
Where does Glimepiride metabolized?
Glimepiride undergoes most of its breakdown in the liver through the activity of the CYP2C9 enzyme, with its byproducts being eliminated from the body via both urine and feces.
Where is Glimepiride manufactured?
Various pharmaceutical companies worldwide produce Glimepiride under brand names and generics in countries, like the U.S., Europe and India.
Where is Glimepiride made?
Manufacturing of products varies depending on the brand or type. With production sites situated in countries like India and Germany alongside hubs such as the U.S.
Where is Glimepiride metabolized?
Your body processes Glimepiride in the liver, mainly using an enzyme called CYP2C9. Once processed, both the active and inactive forms of the drug are removed from your body through your kidneys and bile.
Glimepiride which class of drug?
Glimepiride is, within the group of medications known as sulfonyureas, which function by encouraging the release of insulin from beta cells, in the pancreas.
Why Glimepiride is taken before food?
Having Glimepiride before eating food helps to synchronize its insulin-releasing impact, with the increase in glucose levels after meals, and hence lessens the chance of blood sugar and enhances control of blood sugar levels.
Why Glimepiride is used with metformin?
Glimepiride is often prescribed alongside Metformin to improve blood sugar management by combining their effects; Metformin helps decrease the livers glucose production while Glimepiride boosts insulin release. Providing an approach to controlling glucose levels.
Why Glimepiride is better than Gliclazide?
Glimepiride tends to last in the body and might be stronger, in situations; nevertheless deciding between Glimepiride and Glicazide is influenced by factors unique to the patient such, as kidney function and the risk of low blood sugar levels.
Why Glimepiride cause hypoglycemia?
Glimepiride triggers the release of insulin of blood sugar levels; this can cause an overproduction of insulin and result in blood sugar levels (hypoglycemia, particularly if meals are skipped or physical activity is boosted.
Why is Glimepiride a high risk medication?
Glimepiride is often seen as risky because it can lead to blood sugar levels in older individuals or those, with kidney issues who don't eat consistently.
Will Glimepiride cause weight gain?
Glimepiride can potentially cause weight gain as it boosts insulin activity leading to increased storage in the body; hence, it is advisable to incorporate weight management techniques.
Will Glimepiride lower blood sugar?
Glimepiride is known to reduce blood sugar levels by boosting the release of insulin in the body; doctors often recommend it to individuals with type 2 diabetes to assist in managing their blood glucose levels within the desired range.
Will Glimepiride cause weight loss?
Glimepiride does not lead to weight loss; instead, it has been known to cause weight gain in some people because of its impact on insulin levels.
Will Glimepiride cause diarrhea?
Diarrhea is not an occurrence, with Glimepiride as a side effect; should it happen though it might be mild and resolve on its own. However if it persists seeking evaluation, from a physician is advisable.
Will Glimepiride raise blood pressure?
Glimepiride usually doesn't cause an increase in blood pressure on its own; however, the unregulated blood sugar levels or weight gain linked to its usage might have an impact on blood pressure in the run.
Will Glimepiride cause hair loss?
Hair loss is not typically associated with Glimepiride as a side effect; any thinning of hair noticed while on this treatment could be attributed to causes like diabetes or unrelated conditions.
Does Metformin cause weight loss?
Metformin is known to help with weight loss in individuals who are overweight by enhancing insulin sensitivity and curbing appetite, which can contribute to gradual weight reduction over time.
How to lose weight fast on Metformin?
For results, in shedding weight while taking Metformin medication, it's recommended to pair it with a balanced diet thats mindful of calories intake and incorporate regular exercise routines into your daily regimen. Simply relying on Metformin won't lead to weight loss unless accompanied by lifestyle modifications.
Signs Metformin is working?
Improvements may manifest through fasting and post-meal blood sugar levels, along with a decrease in HbA1c levels and a boost in energy levels; there's also a chance of experiencing weight loss as well as fewer signs of diabetes, such as tiredness or frequent urination.
Does Metformin help with weight loss?
Metformin can assist in weight loss by enhancing insulin sensitivity and reducing glucose output while also curbing appetite; though the impact is typically gradual and modest in nature.
Does Metformin cause diarrhea?
Diarrhea can often occur as an outcome when initiating Metformin treatment; however, it is generally short-lived and diminishes once the body adapts to the medications effects. Aiding with food intake could potentially alleviate discomforts.
Best time to take Metformin?
Metformin is typically recommended to be taken alongside meals such as breakfast or dinner to reduce stomach-related discomfort and improve its absorption by the body.
Foods to avoid while taking Metformin?
Limit the consumption of alcohol and sugary foods while avoiding fatty meals well to reduce the risk of lactic acidosis and potential adverse effects on gastrointestinal health and glucose regulation.
How long does it take for Metformin to work?
Metformin starts to take effect in a few days; its full impact on blood sugar and HbA1c usually becomes noticeable after 4 to 8 weeks of usage.
How does Metformin help you lose weight?
Metformin helps with losing weight by reducing the production of glucose in the liver and enhancing sensitivity to insulin while also curbing hunger cravings. Resulting in calorie consumption and improved metabolic performance.
Why does Metformin cause diarrhea?
Diarrhea can happen because of glucose movement in the intestines and alterations in the gut population, typically occurring more often when starting treatment or increasing the dosage.
Does Metformin help you lose weight?
Metformin can help overweight individuals shed some pounds by enhancing how their bodies process energy and curbing hunger cravings – especially when paired with a diet and regular physical activity.
What is the lowest dose of Metformin you can take?
The initial recommended amount is 500 milligrams a day administered initially to gauge tolerance and minimize digestive discomfort before gradually increasing the dosage above that level.
How long does Metformin take to work?
Metformin begins to reduce blood sugar levels; however, it may take 2 months to see its full impact, on HBA ₁C levels improve significantly with regular usage and healthy lifestyle practices.
Benefits of Metformin?
The advantages encompass management of blood sugar levels and weight maintenance or reduction along with decreased resistance to insulin and shielding of the system as well as possible benefits, in slowing aging and preventing cancer.
Does Metformin make you sleepy?
Sleepiness is not a result of taking Metformin medication; if you experience this symptom while using it could be related to factors, like blood sugar levels, ineffective glucose management or other unrelated issues that need to be assessed.
When is the best time to take Metformin?
The optimal timing for taking this medication is around meal times. Either during or after having breakfast or dinner. It can help minimize stomach discomfort and maintain a blood sugar-lowering effect.
Metformin dosage for weight loss in non diabetics?
Metformin is occasionally prescribed at 500 mg per day for non diabetics off label. Must be monitored by a professional due to possible side effects and risks.
Does Metformin cause weight gain?
Metformin doesn't cause weight gain; in reality, it can actually help prevent weight gain or even lead to weight loss for individuals with insulin resistance.
How long does Metformin stay in your system?
Metformin typically remains in the body for 6 hours before being eliminated within 24 to 48 hours following the final dose based on kidney function.
How long does it take Metformin to work?
It typically begins to reduce blood sugar levels within a days; however, significant improvement in HBA 11C is generally observed after 4 to 3 weeks of usage.
How to take Metformin?
When using metformin, its recommended to have it with meals to lessen any stomach related issues that may occur as effects of the medications intake process, which can be prescribed for twice daily consumption based upon the specific formulation and guidance, from a healthcare provider or doctor; typically extended release tablets are taken during the evening meal, for better efficacy and tolerance.
What happens if you take too much Metformin in one day?
Excessive intake of Metformin can result in stomach-related effects and hypoglycemia (particularly when combined with medications), and in rare cases lactic acidosis may occur – a critical condition necessitating urgent medical attention.
Best time to take Metformin for weight loss?
To enhance weight loss results effectively. Minimize any discomforts in the stomach related to Metformin consumption for weight management purposes it is recommended to take Metformin with meals continuously at the largest meal each day, for sustained effectiveness and appetite control.
What is the lowest dose of Metformin you can take for PCOS?
The usual starting dose for PCOS is 500 mg per day. May be adjusted over time based on how it is tolerated and how effective it is in treating the condition while being monitored by a doctor.
Can Metformin cause diarrhea?
Diarrhea is quite a side effect that often occurs when starting the medication or adjusting the dosage levels; having it with meals and opting for extended-release versions could offer some relief.
What is Metformin used for other than diabetes?
Metformin is not prescribed for type 2 diabetes. Also for PCOS (polycystic ovary syndrome), insulin resistance issues, and prediabetes conditions; occasionally it is even used for weight management or, for antiaging effects, under the guidance of a doctor.
Can I stop taking Metformin when my sugar back to normal?
Stopping Metformin without consulting a healthcare professional is not advisable as it could lead to a decline in blood sugar management when the medication is discontinued and considering diabetes is usually a long-term health concern.
How fast does Metformin work?
Metformin starts to reduce blood sugar levels in 48 hours. The impact on glucose levels becomes noticeable within a week; however, it takes weeks to see improvements in HbA1c levels.
Does Metformin cause constipation?
Constipation is not a result of taking Metformin; however, certain individuals may experience this effect at times. Enhancing the consumption of water and fiber might be beneficial in addressing this concern.
Alternative to Metformin?
Other possible choices consist of medications such as Glipizide, Sitagliptin, Pioglitazone, or SGLT2 inhibitors like Dapagliflozin. The decision is based on factors, like kidney function, heart health risk and financial considerations.
How does Metformin work for weight loss?
Metformin helps lower the production of glucose in the liver and enhances insulin sensitivity while also reducing appetite. These combined effects lead to a decrease in energy intake and gradual weight loss over time.
Can you take Metformin and Ozempic together?
It is safe to use Metformin and Ozempic (Semaglutide) as they work well in improving blood sugar levels and aiding weight loss efforts.
Metformin constipation?
Constipation with Metformin is not very common. Can happen occasionally; usually mild and manageable through increased fluid intake or fiber consumption, or by switching to extended-release versions of the medication.
How long for Metformin to work?
The impact of Metformin typically starts to show within a few days. Its complete blood sugar lowering effects can be seen after using it for 1 to 2 months.
How to stop Metformin diarrhea?
Taking Metformin with meals and opting for the extended release version can help minimize the chances of experiencing diarrhea while starting with a dose and gradually increasing it's advisable to manage any potential side effects effectively; if issues persist despite these measures seeking advice, from a healthcare provider, for alternative treatment options is recommended.
Best time of day to take Metformin?
It's recommended to take Metformin with meals. With breakfast, if taken once a day or with breakfast and dinner if taken daily; being consistent is important.
Can you take Metformin while pregnant?
Indeed Metformin is typically maintained throughout pregnancy for individuals experiencing PCOS or gestational diabetes; nevertheless, its administration ought to be supervised by a healthcare provider, like an obstetrician or endocrinologist.
Can Metformin cause weight gain?
Metformin typically does not lead to weight gain; in fact it might even assist in averting weight gain linked to insulin resistance or other diabetes therapies.
What happens if you take Metformin and don't need it?
Overusing Metformin can cause blood sugar levels and digestive discomfort well as disrupt metabolism; therefore, it's best to avoid taking it unless prescribed by a medical professional.
Can you take berberine with Metformin?
Berberine and Metformin work in ways and could potentially boost each other's benefits; however, combining them may lead to a likelihood of experiencing gastrointestinal side effects and should be managed with caution.
Can you drink on Metformin?
When on Metformin medication ,it's best to avoid or limit alcohol intake since it can heighten the chances of acidosis occurrence. For individuals with kidney or liver issues.
Can Metformin cause constipation?
Constipation happens compared to diarrhea when using Metformin; however, it is possible to experience it occasionally too. Adequate intake of water and fiber in your diet typically assists in addressing this symptom.
Can Metformin cause Fatigue?
Metformin is usually not known to be a cause of exhaustion; Fatigue might arise when blood sugar levels decrease excessively or in uncommon scenarios of vitamin B12 insufficiency or lactic acidosis.
Does Metformin cause kidney damage?
Metformin doesn't lead to kidney harm; however, it should be used carefully in individuals with reduced kidney function as, in these instances the medication may build up and raise the chances of acidosis occurring.
Are Metformin bad for you?
When taken as directed, Metformin is typically safe and efficient, with any negative reactions being minor and easily handle,d posing a risk in instances of severe kidney issues or improper use.
Are Metformin side effects temporary?
Most of the side effects, like feeling sick, in your stomach, or bloating, typically go away after a week of consistent use or adjusting the dosage.
Are Metformin and Ozempic the same?
Metformin and Ozempic are not the kind of medications; Metformin belongs to the biguanide group whereas Ozempic is classified as a GLP-1 receptor agonist medication, with mechanisms of action.
Are Metformin and Ozempic similar?
Lower blood glucose levels and aid in weight loss are two goals pursued by means; Metformin focuses on tackling insulin resistance and reducing liver glucose production while Ozempic works by imitating a gut hormone to boost insulin levels and curb appetite.
Are Metformin and Berberine the same?
Metformin is actually a medication that requires a prescription, whereas Berberine is derived from plants and is considered a supplement of a prescribed drug, like Metformin even though both work to lower glucose levels in different ways.
Can Metformin help with weight loss?
Metformin could potentially aid in steady weight reduction by enhancing sensitivity to insulin and curbing cravings – beneficial for those who are overweight or have insulin resistance issues.
Can Metformin be taken without food?
Taking Metformin without eating is not advisable as it can heighten the chances of experiencing stomach-related issues, like nausea or diarrhea; it's best to have it with food.
Can Metformin cause hypoglycemia?
Metformin doesn't typically lead to blood sugar by itself. The chances go up when used alongside other medications that lower glucose levels, like sulfonylureas or insulin
Can Metformin cause itchy skin?
It's uncommon for itchy skin to occur as a side effect; reactions or a deficiency in vitamin B12 (due to prolonged use of the substance) can lead to skin-related symptoms arising from it. It is advisable for a healthcare provider to assess itching issues.
Can Metformin cause kidney damage?
Metformin doesn't cause harm to the kidneys. It can build up in individuals with kidney issues and result in lactic acidosis. A rare yet severe complication.
How metformin cause lactic acidosis?
Metformin has the potential to affect how mitochondria function and raise the levels of lactate produced in situations; this is particularly notable in individuals with kidney issues or liver and heart problems. May result in lactic acidosis.
How Metformin helps in weight loss?
Metformin helps with losing weight by lowering the production of glucose in the liver and enhancing insulin sensitivity while also slightly curbing appetite to help maintain a deficit.
How Metformin causes vitamin B12 deficiency?
Prolonged use of Metformin could potentially hinder the absorption of vitamin B12 in the intestines by impacting calcium membrane transport mechanisms, resulting in a deficiency developing gradually over time.
What Metformin does to the body?
Metformin reduces blood sugar levels by slowing down the livers glucose production process and increasing sensitivity to insulin while enhancing glucose absorption in muscles; additionally, showcasing impacts on lipid levels and body weight management.
When Metformin should be taken?
It's recommended to take Metformin with meals, like breakfast and/or dinner to enhance absorption and lower the chances of experiencing issues.
When Metformin is contraindicated?
Metformin should not be used in individuals with kidney issues (when eGFR is below 30 mL/min), metabolic acidosis present or situations involving a risk of oxygen levels, like severe infections or surgery.