Rifampicin
- I. Introduction
- II. Composition of Rifampicin
- III. How Rifampicin Works
- IV. Uses of Rifampicin
- V. Dosage and Administration
- VI. Interaction of Rifampicin
- VII. Side Effects of Rifampicin
- VIII. Warnings and Contraindications
- IX. Careful Administration of Rifampicin
- X. Special Considerations for Administration
- XI. Overdose of Rifampicin
- XII. Storage and Handling Precactions for Rifampicin
- XIII. Important Precautions for Rifampicin Use
I. Introduction
A. Brief Overview of Rifampicin
Rifampicin, a proper antibiotic, is a crucial component of antimicrobial treatment for a variety of infectious illnesses. It has bacteria-killing properties, especially against bacteria that grow slowly or remain dormant. This makes it extremely valuable in the fight against tuberculosis and leprosy.
B. History and Development of Rifampicin
The origins of Rifampicin can be traced back to the 1950s when scientists working at Gruppo Lepetit SpA discovered it in a soil bacterium called Streptomyces mediterranei. In the 1960s, its effectiveness in fighting Mycobacterium tuberculosis, the bacteria responsible for causing tuberculosis, became evident due to its antimicrobial properties.
C. Role of Rifampicin in Modern Medicine
Rifampicin remains a component of modern medicine, with its significant effects in treating tuberculosis and leprosy. Additionally, it is utilized for preventing meningitis and treating infections. Moreover, Rifampicin's effectiveness also extends to managing conditions like endocarditis, osteomyelitis, and prosthetic joint infections. This demonstrates its role in current therapeutic practices.
II. Composition of Rifampicin
A. Chemical Composition and Structure
Rifampicin is classified as an antibiotic within the rifamycin family. The unique chemical makeup of Rifampicin, consisting of a naphthohydroquinone core combined with a depsipeptide, plays a role in its powerful antibacterial properties. Additionally, the molecule contains an ansa chain, a characteristic feature of the rifamycin group, and contributes to its ability to dissolve in fats.
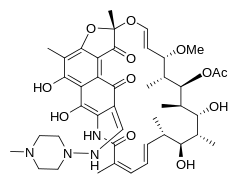
B. Pharmaceutical Forms and Strengths
Rifampicin is available in forms and strengths to meet the needs of various patients. It is commonly sold as capsules, tablets, and injectable solutions. The oral versions usually come in strengths of 150mg and 300mg, while the injectable form is found in vials of 600mg. In some areas, Rifampicin is also combined with antitubercular medications in fixed-dose combinations to make it easier for patients to take and improve their adherence to treatment.
III. How Rifampicin Works
A. Mechanism of Action
Rifampicin works by blocking the activity of RNA polymerase, an essential enzyme responsible for converting DNA into RNA. It does this by interacting with a part of the enzyme preventing it from starting the transcription process. As a result, bacterial protein production is. Their growth is inhibited. The reason Rifampicin targets bacteria more than humans is because it has an affinity for bacterial RNA polymerase compared to the human version, which explains its selective toxicity towards bacterial cells.
B. Impact on Bacterial Cells
The use of Rifampicin causes a halt in the growth and reproduction of cells by interrupting protein synthesis. This incredibly impacts growing or dormant bacteria like those found in the Mycobacterium species. Rifampicin plays a role in treating chronic or latent infections, such as tuberculosis, where bacteria can remain inactive for extended periods. Moreover, Rifampicin's strong ability to kill bacteria also makes it effective in eradicating bacteria inside host cells, making it essential for combating infections.
IV. Uses of Rifampicin
A. Official Uses in Medicine
Rifampicin, an antibiotic, is commonly prescribed to address bacterial infections. It is often combined with antibiotics like pyrazinamide, isoniazid, and ethambutol for effective tuberculosis (TB) treatment. Additionally, rifampicin is utilized in treating leprosy and Legionnaires disease123.
Here are some references for you to check out:
1: Rifampicin - Wikipedia 2: Guidelines for the Diagnosis, Treatment, and Prevention of Leprosy 3: Package leaflet: Information for the patient Rifampicin 300 … - medicines
B. Off-label Uses
Rifampicin has been utilized off-label to provide protection against meningitis12 and has been employed in treating infections34.
Here are some references for you to check out:
1: Treatment and prevention of meningococcal infection - UpToDate 3: Rifampin Uses, Side Effects & Warnings - Drugs.com 2: Control and Prevention of Meningococcal Disease: Recommendations of the … - CDC 4: Rifampicin - Wikipedia
V. Dosage and Administration
A. Standard Dosage Guidelines
The recommended amount of Rifampicin can differ depending on the purpose it serves. In the case of treating tuberculosis, adults usually take 600mg once a day, whereas children's dosage is adjusted based on their weight, typically ranging from 10 20mg per kilogram per day. When managing leprosy, it is common to administer a monthly dose of 600 mg of Rifampicin. However, these guidelines may be modified based on clinical situations and should be tailored by a healthcare professional.
B. Dosage Adjustments Based on Specific Factors
In some cases, adjustments may be needed in the usual dosage of Rifampicin. This is particularly relevant for patients with liver problems, as the dose may need to be lowered or used cautiously. Factors such as age, weight, and kidney function can also play a role in determining the appropriate dosage. As a result, healthcare professionals should carefully evaluate these factors before prescribing Rifampicin. Make any necessary adjustments to the dose.
C. Method of Administration
Rifampicin is usually taken by mouth. It's recommended to take it when your stomach is empty. It's best to take it one hour before or two hours after a meal to make sure your body absorbs it properly. If you have difficulty taking medications, you can also receive Rifampicin through an intravenous formulation. No matter which way you take it, following the dosage schedule is extremely important for the treatment to work effectively and to avoid the development of drug resistance.
VI. Interaction of Rifampicin
A. Drug-Drug Interactions
Rifampicin is well known for its ability to interact with drugs. It can significantly influence the levels of medications in the bloodstream by activating liver enzymes responsible for drug metabolism. This interaction is particularly relevant for drugs like warfarin contraceptives and specific antivirals. As a result, when taking Rifampicin along with these medications, it may be necessary to adjust dosages or closely monitor their effects.
B. Drug-Food Interactions
Absorption of Rifampicin when taken orally may be affected by food, especially meals high in fat. Hence it is recommended to take the medication on a stomach. Besides this, there are no interactions between Rifampicin and food. However, it is advisable to limit alcohol intake during treatment to avoid liver damage.
C. Impact on Laboratory Tests
Rifampicin can potentially disrupt laboratory tests, which can result in inaccurate outcomes. One notable effect is the possibility of urine, sweat, and tears turning orange, which may interfere with urine testing. Furthermore, it can temporarily affect liver function test results, so interpreting these findings when patients undergo Rifampicin therapy is essential.
VII. Side Effects of Rifampicin
A. Common Side Effects
Gastrointestinal Issues; These consist of nausea, throwing up, discomfort in the abdomen, and loss of appetite. The majority of these symptoms are usually mild. Tend to improve as the treatment progresses. Skin-related Reactions; Mild skin rashes, itching, and flushing are some side effects that may occur with the use of Rifampicin. However, rare severe reactions, like Stevens-Johnson syndrome, can sometimes happen.
B. Serious Side Effects
Rifampicin can potentially cause harm to the liver ranging from increases in liver enzyme levels without symptoms to severe liver failure. It is advised to monitor liver function tests during treatment, especially in patients with liver disease. However, rare severe allergic reactions, like angioedema or anaphylaxis, can occur as side effects. If these reactions are observed, stopping the medication and seeking appropriate medical attention is essential.
C. Long-term Side Effects
Extended use of Rifampicin may have the potential to result in severe side effects. These include hepatitis, interstitial nephritis, and hematologic irregularities like thrombocytopenia and eosinophilia. Hence it is crucial to observe patients undergoing long-term Rifampicin treatment for these harmful impacts.
VIII. Warnings and Contraindications
A. General Warnings for Rifampicin Use
It is essential to use Rifampicin due to its potential to cause liver damage. It is regularly monitoring liver function tests before, during, and after the treatment is recommended. Additionally, patients should be informed about the reddish-orange discoloration of bodily fluids that may occur. Rifampicin has properties that can affect the effectiveness of other medications taken at the same time. Therefore, assessing any possible interactions with other drugs while undergoing Rifampicin therapy is crucial.
B. Contraindications for Specific Populations
Patients with liver disease should not take Rifampicin because it can worsen their liver problems. If they take this medication, it is essential to monitor patients with mild to moderate liver impairment. If someone has experienced hypersensitivity reactions to Rifampicin or its components, they should avoid using it. Signs of hypersensitivity may include itching, difficulty breathing, or swelling of the face, lips, or tongue.
IX. Careful Administration of Rifampicin
A. Importance of Adherence to Dosing Schedule
It is crucial to follow the recommended dosing schedule for treatment. Taking medications irregularly can result in drug levels, which can decrease effectiveness and contribute to the development of drug resistance. Therefore, advising patients about adhering to their prescribed dosing regimen is important.
B. Monitoring for Adverse Reactions
Monitoring for any potential adverse effects when undergoing Rifampicin treatment is crucial. This involves getting tests to check liver function, complete blood counts, and evaluate kidney function. If any significant adverse reactions occur, adjusting the dosage or even stopping the treatment may be necessary.
C. Management of Missed Doses
If you forget to take a dose, try to take it soon as you remember. However, if it's almost time for your dose, it's best to skip the missed dose and continue your regular dosing schedule. It's essential not to take doses as this can lead to an overdose.
X. Special Considerations for Administration
A. Administration to Elderly Patients
Elderly individuals may need to carefully adjust their medication dosage and receive monitoring while undergoing Rifampicin treatment. This is due to the possibility of age-related decline in liver, kidney, or heart function well, as any existing medical conditions or concurrent use of other medications.
B. Administration to Pregnant Women and Nursing Mothers
Rifampicin should only be used during pregnancy if the benefits outweigh the risks to the baby. It is essential to be cautious when giving Rifampicin to breastfeeding mothers because it can be present in breast milk. Talking with a healthcare provider about weighing the risks and benefits is recommended.
C. Administration to Children
Rifampicin has been authorized for use in children, even newborns. However, determining the dosage typically relies on the child's weight. Observing any potential side effects and therapeutic outcomes is crucial, mainly due to the potential risk of liver toxicity.
XI. Overdose of Rifampicin
A. Symptoms of Overdose
Experiencing an intake of Rifampicin can lead to various symptoms, such as nausea, vomiting, abdominal discomfort, itchiness, headaches, and fatigue. In severe cases, it can cause liver problems indicated by yellowing of the skin and elevated liver enzymes, sudden kidney failure, and difficulty breathing. In some situations, one may even lose consciousness or have seizures. If there is any concern about an overdose, it is crucial to seek immediate medical assistance.
B. Treatment and Management of Overdose
The primary approach to managing an overdose of Rifampicin is mainly supportive and symptomatic, focusing on maintaining bodily functions. This might involve procedures like lavage, using activated charcoal, and implementing general measures to provide support. In severe cases with significant liver damage, specific treatment may be necessary. While hemodialysis can be considered for overdose situations, it's important to note that its effectiveness in removing Rifampicin from the body is limited.
XII. Storage and Handling Precactions for Rifampicin
A. Proper Storage Conditions
Rifampicin needs to be stored at a temperature range of 20°C to 25°C (68°F to 77°F), which is considered room temperature. Keeping it from heat, moisture, and direct light is essential. Remember to store all medications where children cannot reach them, as this helps prevent ingestion.
B. Safe Handling Instructions
It is important not to crush or chew rifampicin capsules; instead, they should be swallowed whole with liquid. Remember to wash your hands after handling the medication. Avoid contact with any crushed or broken tablets, as rifampicin may temporarily cause a discoloration (red-orange) of the skin.
XIII. Important Precautions for Rifampicin Use
A. Prevention of Drug Resistance
Inconsistent usage of Rifampicin can result in the emergence of drug resistance, which poses a concern in treating tuberculosis. It is essential to adhere to the treatment course, even if symptoms improve, to prevent the development of resistant strains. Medical professionals usually prescribe Rifampicin as part of combination therapy.
B. Potential for Drug-Induced Hepatitis
Although it is uncommon, Rifampicin has the potential to cause drug-induced hepatitis, especially when taken in doses or by individuals with existing liver conditions. To ensure safety, it is advised to monitor liver function tests during treatment. If any symptoms of liver damage such as nausea, vomiting, abdominal pain, or jaundice occur, it is crucial to discontinue Rifampicin and seek guidance from a healthcare professional.
C. Risk of Red-Orange Body Fluids
Rifampicin has been observed to result in a reddish-orange coloration of fluids such as sweat, tears, urine, and feces. Although this is harmless, it's worth noting that it can potentially stain clothing and contact lenses. Patients must be aware of this effect to avoid any unnecessary concern if they encounter it unexpectedly.